Comprehensive Cancer Prevention Toolkit for Clinicians
You can use the Comprehensive Cancer Prevention Toolkit for Clinicians in your daily practice to make cancer prevention easier and more effective. The toolkit gives you practical tools and guides based on proven research. These resources help you bridge the gap between knowledge and action. You get access to strategies that reduce cancer risk for your patients. Take steps today to improve outcomes and deliver care that makes a real difference.
Key Takeaways
Utilize the Comprehensive Cancer Prevention Toolkit to enhance cancer prevention in your practice. It provides practical tools and strategies based on proven research.
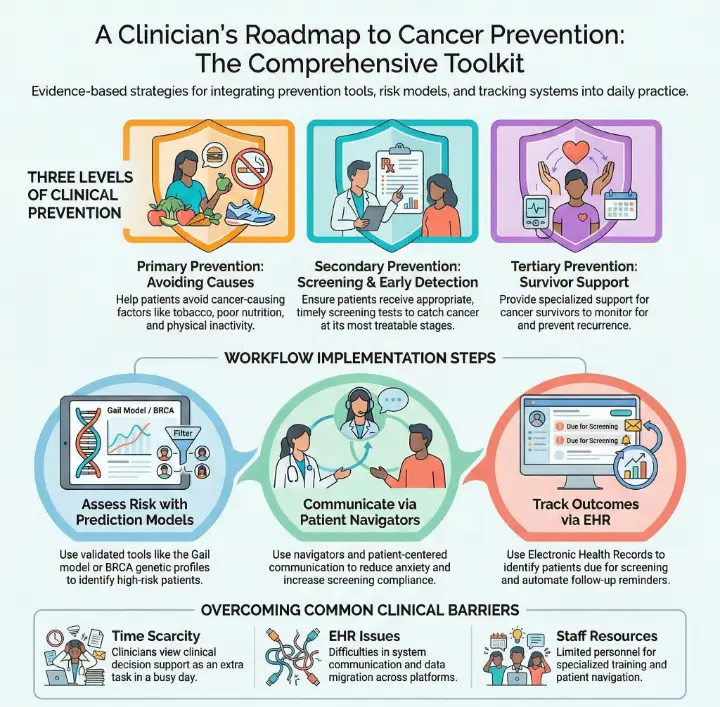
Focus on three main areas of prevention: primary (avoiding cancer causes), secondary (screening tests), and tertiary (supporting cancer survivors). Prioritize primary prevention for the best outcomes.
Engage patients through effective communication methods. Use patient navigators, reminders, and educational materials to ensure they understand cancer risks and prevention strategies.
Implement a tracking system to monitor patient screenings and follow-ups. Use EHRs to identify patients due for screenings and send reminders to improve compliance.
Continuously evaluate and improve your cancer prevention efforts. Regularly review data, share results with your team, and adjust strategies based on what works best.
Toolkit Overview and Key Resources

Main Components for Clinical Practice
You can find several important resources in the Comprehensive Cancer Prevention Toolkit for Clinicians. These resources help you plan, deliver, and improve cancer prevention in your practice. The CDC Program Evaluation Toolkit stands out as a key tool. It guides you through six steps for planning and evaluating your cancer prevention efforts. The toolkit encourages you to work with others, focus on equity, and use what you learn to make your program better.
Component | Description |
|---|---|
Six Steps | Shows you how to plan and carry out program evaluation. |
Engage Collaboratively | Helps you work with partners for better results. |
Advance Equity | Makes sure everyone has a fair chance at cancer prevention. |
Learn from Insights | Lets you use feedback to improve your strategies. |
You can also use clinical practice algorithms, which give you clear steps for screening and managing patients. The Readiness Assessment Planning Guide helps you check if your clinic is ready to use new cancer prevention methods.
Evidence-Based Tools and Guides
The Comprehensive Cancer Prevention Toolkit for Clinicians includes guides that many experts recommend. These guides help you increase cancer screening rates and improve care quality. For colorectal cancer, you can use action guides and toolkits developed by the CDC and partners.
Title | Source |
|---|---|
Increasing Colorectal Cancer Screening and Promoting Screening Quality | CDC’s Division of Cancer Prevention and Control |
Increasing Colorectal Cancer Screening: An Action Guide for Working with Health Systems | CDC’s Division of Cancer Prevention and Control |
Health Systems Improvement Toolkit: A Guide to Cancer Screening in Indian Country | CDC and National Indian Health Board |
You can also use the WHO Cervical Cancer Prevention and Control Costing Tool to plan and budget for cervical cancer programs. These resources help you reach more patients and improve health for everyone. When you use evidence-based tools, you can prevent more than half of cancers, especially by focusing on nutrition, physical activity, and tobacco use. Community partnerships make your efforts even stronger.
Tip: Federally Qualified Health Centers can use these resources to reach people who face health disparities.
How to Use the Comprehensive Cancer Prevention Toolkit for Clinicians
You can make cancer prevention part of your daily routine by following a few clear steps. The Comprehensive Cancer Prevention Toolkit for Clinicians gives you a path to follow. You can use it to assess risk, apply prevention strategies, educate patients, and track progress. Here is how you can use the toolkit in your practice.
Assessing Patient Risk
Start by finding out which patients have a higher chance of getting cancer. You can use validated risk prediction tools to help with this. These tools use information about family history, genetics, and lifestyle. Some examples include:
Cancer risk prediction models that show a person’s chance of getting cancer and help find genetic risks, like BRCA 1 or BRCA 2.
New models that use genetic profiles and information about the environment.
The NCI colorectal cancer risk tool and the Gail breast cancer risk model, which you can use in primary care.
These tools help you and your patients understand their risk. They also help patients make better choices about screening and prevention. You do not need to worry about causing anxiety. Studies show that these tools improve knowledge and encourage screening.
Tip: Use these tools with every patient, not just those with a family history of cancer.
Applying Prevention Strategies
Once you know a patient’s risk, you can use the toolkit to guide your next steps. Cancer prevention works best when you focus on three main areas:
Primary prevention: Help patients avoid things that cause cancer. This includes stopping tobacco use, eating healthy foods, staying active, and avoiding harmful chemicals.
Secondary prevention: Make sure patients get the right screening tests. Early detection can save lives.
Tertiary prevention: Support patients who have had cancer to prevent it from coming back.
You should focus on primary prevention first. Many cancer deaths happen because of tobacco, poor diet, and lack of exercise. You can help patients make better choices by giving them resources and support. The Comprehensive Cancer Prevention Toolkit for Clinicians has guides and action plans for each type of prevention.
Patient Education and Communication
Good communication helps patients understand cancer prevention. You can use several methods to make your message clear:
Patient navigators who guide patients through the process.
Reminders by phone, mail, or email.
Small media like posters, brochures, or automated calls.
Training for providers to improve communication skills.
Patient-centered communication that listens to patient concerns and involves them in decisions.
You can also use a genetics toolkit to collect family history and refer patients for genetic counseling. When you give strong recommendations, patients are more likely to get vaccines like HPV and complete the series. Patient-centered communication increases the chance that patients will get screened. Always answer questions and involve patients in their care.
Note: Use simple language and check that patients understand the information.
Tracking and Follow-Up
You need a system to keep track of patients and make sure they get the care they need. The toolkit suggests these steps:
Component | Description |
|---|---|
Identify patients due for screening tests | Use your EHR or other systems to find patients who need screening. |
Develop and send reminder | Choose how to remind patients (call, email, mail) and check contact details. |
Track outcomes | Follow patients through screening and diagnostic tests. |
Partnerships | Work with partners inside and outside your clinic. |
Staff | Make sure you have support to manage reminders and results. |
You can also work with patient navigators, social workers, or community health workers. Set up a process to monitor your system and track outcomes. This helps you see what works and where you can improve.
Callout: Adapting resources for diverse groups makes your program stronger. Use community outreach to reach more people and address health equity.
The Comprehensive Cancer Prevention Toolkit for Clinicians fits into your workflow. You can use it to guide every step, from risk assessment to follow-up. This approach helps you reach more patients and improve cancer prevention in your practice.
Integrating the Toolkit into Workflow
Seamless Adoption Tips
You can make cancer prevention part of your daily routine by planning ahead. Start by reviewing the Comprehensive Cancer Prevention Toolkit for Clinicians with your team. Assign clear roles so everyone knows their tasks. Use checklists to track progress. Set up regular meetings to talk about what works and what needs to change.
Tip: Make patient information easy to access for all staff. This helps everyone stay on the same page.
To address diversity, equity, inclusion, and justice (DEIJ), you can:
Create a DEIJ Task Force in your clinic.
Use training that follows National Culturally and Linguistically Appropriate Services (CLAS) Standards.
Offer patient materials in different languages.
Collect and review data about your patients’ backgrounds.
Give staff training on recognizing and reducing bias.
Using EHRs Effectively
Electronic Health Records (EHRs) help you organize and improve cancer prevention. EHRs can connect your clinic to national and regional data. This supports research and helps you learn from others. You can use EHRs to:
Set up reminders for cancer screenings, like colonoscopies and mammograms.
Use tools that combine patient health data with clinical information. For example, MeTree helps you find patients who need more screening or genetic testing.
Track which patients need follow-up care.
Share information with other clinics and research programs.
EHRs also let you send nudges to both clinicians and patients. These reminders increase the number of people who get screened. When you use EHRs well, you can spot patients at higher risk and help them sooner.
Team-Based and Multidisciplinary Care
Working as a team makes cancer prevention stronger. You can bring together doctors, nurses, social workers, and patient navigators. Each person adds a different skill. When you work together, you find barriers and solve problems faster. This approach helps you reach more patients and improve cancer outcomes.
A team-based model also supports DEIJ. You can share ideas and learn from each other. Regular meetings help everyone stay focused on patient needs. When you use the toolkit as a team, you deliver better care and help more people stay healthy.
Overcoming Barriers in Practice
Managing Time and Resources
You face many challenges when you try to use cancer prevention toolkits. Time and staff resources often create the biggest obstacles. Many clinicians struggle to fit new protocols into busy schedules. You may see more patients each day, which leaves little time for extra tasks. Staff training and communication also take time. The table below shows common barriers you might encounter:
Barrier Type | Description |
|---|---|
EHR issues | Difficulties in using EHR systems, including communication and data migration problems. |
Staff resources, including time | Limited staff time and resources for training and implementation. |
Competing priorities | Other urgent patient needs make it hard to focus on cancer prevention. |
Staff buy-in | Some staff resist changes in protocol. |
Training needs | Training information does not reach all staff, especially non-clinical members. |
Communication | Meetings and coordination among staff can be challenging. |
Complexity of intervention training | Training for preventive interventions can be complex. |
Clinician motivation | Some clinicians lack motivation to use new protocols. |
Sustainable funding | Financial constraints limit program maintenance. |
You may also notice that time is the scarcest resource. Many clinicians see clinical decision support as another task in a busy day. The push to increase patient visits makes it harder to adopt new practices.
Evidence Description | Key Points |
|---|---|
PCPs view CDS as another initiative | CDS can feel like an extra burden for overworked clinicians. |
Increased patient load | More patient visits each day create barriers for new protocols. |
Clinician time is limited, making integration difficult. |
Tip: Use checklists and simple reminders to save time and keep your workflow efficient.
Engaging Patients and Communities
You can reach more patients by working with your community. Community outreach helps you share cancer prevention messages and build trust. You may use local events, health fairs, or partnerships with schools and faith groups. Culturally relevant education programs improve health literacy and encourage wellness. When you involve patients and families, you make prevention easier to understand.
Host cancer education sessions in your community.
Share materials in different languages.
Work with community leaders to promote screening and healthy habits.
Callout: Community engagement increases early detection and helps reduce health disparities.
Solutions for Limited Support
If you have limited resources, you can still help your patients. Many organizations offer free support and services. You can connect patients to these options:
Patient navigation services guide patients through care.
Financial and insurance support helps patients manage costs.
Free rides and lodging make treatment easier for those who travel.
Smoking cessation programs support healthy choices.
A 24/7 cancer helpline answers questions and provides guidance.
You can also build partnerships with local groups and use online resources. These solutions help you overcome barriers and deliver better cancer prevention.
Measuring Success and Improving Outcomes

Monitoring and Evaluation
You need to know if your cancer prevention efforts work. You can use simple tools to measure your progress. Start by tracking how many patients get screened and how many follow prevention advice. You can use surveys before and after your interventions to see if patients understand cancer risks better. Community Health Workers (CHWs) help you reach more people and make them feel comfortable with screening. When you use CHWs, you often see more patients getting screened and learning about cancer risks.
You can use these methods to measure success:
Track changes in patient knowledge about cancer risk factors.
Count how many patients complete cancer screenings.
Use focus groups to learn how patients feel about your program.
Methodology | Findings |
|---|---|
Statistical Tests (t-tests, chi-square) | Show improved cancer awareness after your interventions. |
Pre-and Post-Intervention Surveys | Reveal more correct answers about cancer risks and prevention. |
Screening Rates | Show more patients getting screened after you start your program. |
You can also use the Provider Reminder Planning Guide. This tool helps you see if providers recommend screenings and if patients complete them. Performance measures let you check both the process and the results. Systematic reviews show that reminders increase screening rates and help you use resources wisely.
Tip: Regular monitoring helps you find what works and what needs to change.
Continuous Improvement Strategies
You can make your cancer prevention program better over time. The CDC Program Evaluation Toolkit gives you a step-by-step way to review your efforts. This toolkit helps you find strengths and areas to improve. When you use evaluation in your program, you make better decisions and help more patients.
You should:
Review your data often.
Share results with your team.
Adjust your strategies based on what you learn.
Celebrate small wins and keep looking for ways to improve.
The CDC Program Evaluation Framework helps you use your findings to guide your next steps. This leads to stronger cancer prevention and better outcomes for your patients.
Note: Continuous improvement means you never stop learning and growing in your practice.
You can make cancer prevention easier by using the toolkit in your daily practice. Start with risk assessment, apply prevention strategies, educate patients, and track progress. You improve patient outcomes and simplify your workflow. Explore these resources for more support:
Cancer Prevention & Screening Guidelines
HPV Vaccination Resources
Cancer Prevention Program for lifestyle changes and early detection
Take action today. Use these tools to help your patients stay healthy.
FAQ
How do I access the Comprehensive Cancer Prevention Toolkit for Clinicians?
You can find the toolkit online through trusted sources like the CDC, American Cancer Society, or your health system’s resource portal. Most resources are free and easy to download.
Can I use the toolkit with all patient populations?
Yes. You can adapt the toolkit for different ages, backgrounds, and risk levels. Many guides include materials in multiple languages and formats for diverse groups.
What if my clinic has limited staff or time?
You can start small. Use checklists and reminders to save time. Focus on one prevention strategy first. Involve your team and use community partners for support.
Tip: Assign one staff member to lead toolkit activities.
How often should I update my cancer prevention strategies?
You should review your strategies at least once a year. Check for new guidelines and resources. Regular updates help you provide the best care for your patients.
This article is for educational purposes only and is not a substitute for professional medical advice. For more details, please see our Disclaimer. To understand how we create and review our content, please see our Editorial Policy.
See Also
An In-Depth Overview of Various Cancer Types
Recognizing Symptoms and Treatment Options for Duodenal Cancer
Identifying Symptoms and Treatment Strategies for Conjunctival Melanoma

