Emerging Biologics A New Hope for Metastatic Cancers
You may hear doctors talk about new treatments called biologics. These are advanced medicines made from living cells. They work differently from older cancer treatments. Many people with metastatic cancer face tough odds. Five‑year survival has improved for some metastatic cancers (like melanoma and lung cancer), but many metastatic cancers still have poor long‑term survival. Experts predict that more people will get cancer in the coming years. Emerging Biologics: A New Hope for Metastatic Cancers brings a fresh approach. These new therapies give you and your loved ones reasons to feel hopeful about the future.
Key Takeaways
Biologics are advanced cancer treatments made from living cells. They target cancer cells more precisely than traditional therapies.
These therapies can improve survival rates and quality of life by focusing on individual cancer characteristics and boosting the immune system.
Emerging biologics include immunotherapy, monoclonal antibodies, and CAR T-cell therapy, each offering unique benefits for different cancer types.
Biologics often cause different and sometimes fewer side effects than chemotherapy, but they can still lead to serious immune‑related reactions.
Personalized medicine is key; doctors will match biologics to your specific cancer, enhancing treatment effectiveness and hope for recovery.
Emerging Biologics: A New Hope for Metastatic Cancers

What Are Biologics
You may wonder what makes biologics different from other cancer treatments. Biologics are special medicines made from living cells. Scientists design them to target cancer in new ways. These treatments can use proteins, antibodies, or even your own immune cells. You might hear about therapies like ado-trastuzumab emtansine, olaparib, sevabertinib, pembrolizumab, Amtagvi, and CAR T-cell therapy. Each one works by focusing on the unique features of cancer cells or by helping your immune system fight cancer.
Emerging Biologics: A New Hope for Metastatic Cancers stands out because these therapies offer a more personal approach. Doctors can match the right biologic to your specific cancer. This shift means you get treatments that fit your needs better than ever before.
Biologics vs. Traditional Treatments
You may know about chemotherapy and radiation. These older treatments attack both cancer and healthy cells. This can cause side effects like hair loss and nausea. Biologics work differently. They aim to target only cancer cells or boost your immune system to fight cancer.
Here is a simple table to help you see the differences:
Treatment Type | Mechanism of Action | Outcomes and Effectiveness |
|---|---|---|
Chemotherapy | Uses drugs that attack fast-growing cells, including healthy ones. | Shrinks tumors but often causes side effects like hair loss and nausea. |
Immunotherapy | Helps your immune system find and destroy cancer cells. | Can lead to long-term remission and better survival, especially in cancers like melanoma and lung cancer. |
Combination Therapy | Mixes chemotherapy and immunotherapy for stronger results. | Improves survival rates in some metastatic cancers. |
You can see a big change in cancer care. Many new treatments focus on your unique cancer. Some examples include:
Antibody therapies like envafolimab and durvalumab for advanced cancers.
Small molecules such as trametinib for melanoma.
Tumor-infiltrating lymphocytes, which use your own immune cells.
Bispecific CAR T cells for blood cancers.
Oncolytic viruses that attack cancer cells directly.
Emerging Biologics: A New Hope for Metastatic Cancers brings you closer to treatments that are safer and more effective. You now have more options that fit your needs and give you hope for the future.
How Biologics Work
Targeting Cancer Cells
You may wonder how biologics find and attack cancer cells. These treatments use natural molecules from your body or ones made in a lab. Scientists design them to spot cancer cells and leave healthy cells alone. Monoclonal antibodies act like smart missiles. They attach to cancer cells and mark them for destruction. Some biologics change how cancer cells grow, making them behave more like healthy cells. Others stop cancer cells from spreading to new places in your body.
Emerging Biologics: A New Hope for Metastatic Cancers uses several methods to target cancer. You see therapies that make cancer cells easier for your immune system to recognize. Some biologics block the process that turns normal cells into cancer cells. You also find treatments that reduce damage to healthy cells compared to older therapies.
Tip: Biologics can prevent cancer cells from hiding, making them easier for your immune system to attack.
Here are some ways biologics target cancer cells:
Marking cancer cells so your immune system can find them.
Stopping cancer cells from growing and dividing.
Preventing cancer cells from spreading.
Boosting the Immune System
Your immune system acts as your body's defense team. Biologics help your immune cells fight cancer more effectively. Checkpoint inhibitors remove the brakes from your immune system, allowing it to attack cancer cells. CAR T-cell therapy uses your own T cells. Doctors change these cells in a lab and send them back into your body to hunt down cancer.
Your immune system includes several types of cells:
B cells make antibodies that attack cancer.
T cells destroy cancer cells directly and signal other cells to help.
Natural killer cells release chemicals to kill cancer.
Monocytes swallow and digest cancer cells.
Biologics boost the power of these cells. Some therapies use cancer vaccines or oncolytic viruses to train your immune system. You gain a stronger defense against cancer with these new treatments.
Emerging Biologics: A New Hope for Metastatic Cancers brings you therapies that work with your body, not against it. You get treatments that help your immune system fight cancer in smarter ways.
Types of Emerging Biologic Therapies
You see many new biologic therapies changing how doctors treat metastatic cancers. These therapies use your body's own cells or special proteins to fight cancer. Each type works in a unique way. You can learn about the most common and promising options below.
Immunotherapy
Immunotherapy helps your immune system find and destroy cancer cells. You may hear about immune checkpoint inhibitors. These medicines block proteins like PD-1, PD-L1, and CTLA-4. When you use these therapies, your immune cells attack cancer more strongly. Doctors use immunotherapy for melanoma, lung cancer, and bladder cancer. You can see improved survival rates, especially in melanoma. About 20 to 40% of patients with advanced melanoma have long-lasting responses.
Here is a table showing how immunotherapy works and its results:
Type of Immunotherapy | Mechanism of Action | Clinical Results |
|---|---|---|
Immune Checkpoint Inhibitors | Block proteins that slow down immune response | Extended survival rates in melanoma and lung cancer; five-year survival rates improved. |
CAR-T Cell Therapy | Changes T cells to better detect cancer | Remission in up to 90% of children and young adults with leukemia. |
Cancer Vaccines | Teach immune system to recognize cancer | Better understanding of tumor antigens is improving effectiveness. |
Monoclonal Antibodies | Attach to cancer cells and signal immune attack | Target many cancers, leading to improved outcomes. |
Note: Immunotherapy gives you hope for long-term remission and better quality of life.
Monoclonal Antibodies
Monoclonal antibodies are lab-made proteins that target cancer cells. You receive these medicines through an IV. They attach to markers on cancer cells and help your immune system destroy them. Doctors use monoclonal antibodies for melanoma, lung cancer, head and neck cancer, cervical cancer, and urothelial carcinoma. PD-1 and PD-L1 inhibitors are now standard for advanced cases.
Here is a table showing where monoclonal antibodies make a difference:
Indication | Comments |
|---|---|
Melanoma | Improved survival rates |
Non-Small Cell Lung Cancer | Standard for advanced cases |
Head and Neck Cancer | Effective in recurrent or metastatic disease |
Cervical Cancer | Useful for advanced or recurrent carcinoma |
Urothelial Carcinoma | Helps patients who cannot get chemotherapy |
Doctors also use antibody-drug conjugates. These combine antibodies with cancer-killing drugs. Sacituzumab govitecan targets Trop-2, a protein found in many cancers. It delivers a drug directly to cancer cells, causing them to die while sparing healthy cells. Fam-trastuzumab deruxtecan-nxki is another example. It treats HER2-low breast cancer and helps patients who do not respond to hormone therapy.
Tip: Monoclonal antibodies offer targeted treatment, reducing side effects and improving outcomes.
CAR T-Cell Therapy
CAR T-cell therapy uses your own immune cells to fight cancer. Doctors take your T cells, change them in a lab, and return them to your body. These cells now recognize and attack cancer. You see this therapy used for blood cancers like leukemia and lymphoma. CAR T-cell therapy has helped up to 90% of children and young adults with leukemia achieve remission.
Here is a chart showing response rates in recent CAR T-cell trials:
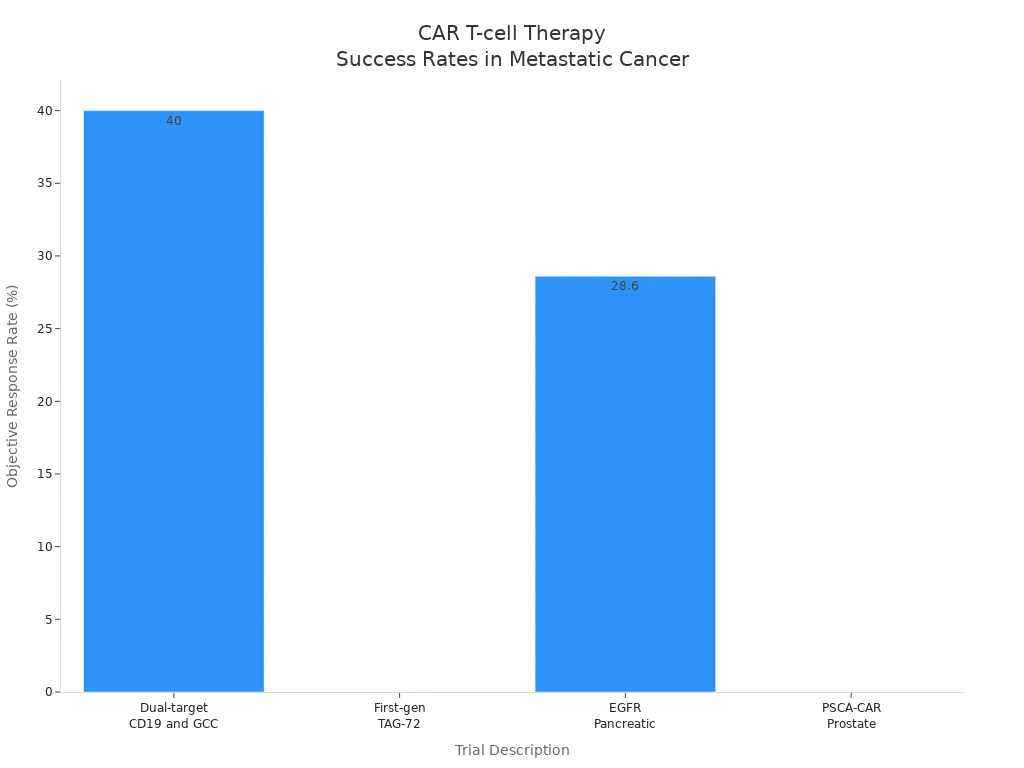
Doctors are testing CAR T-cell therapy for solid tumors like pancreatic and prostate cancer. Some trials show response rates of 28.6% in pancreatic cancer. You may see more options as research continues.
Alert: CAR T-cell therapy is highly personalized. Your treatment is made just for you.
Bispecific Antibodies
Bispecific antibodies are new medicines that can attach to two targets at once. One part binds to cancer cells. The other part connects to immune cells. This brings your immune cells closer to cancer, making it easier to attack. Doctors use bispecific antibodies and CAR T‑cell therapies for blood cancers like acute lymphoblastic leukemia, and bispecific CAR‑T approaches are being studied in trials.
Innovative approaches help you stay safe during treatment. You may use home monitoring tools like blood pressure cuffs and thermometers. You receive educational materials to track symptoms. A team of doctors, nurses, and pharmacists works together to support you.
Innovative Approach | Description |
|---|---|
You measure vital signs at home. | |
Educational Resources | You get wallet cards and booklets to track symptoms. |
Multidisciplinary Team | A group of healthcare providers supports your care. |
Note: Bispecific antibodies offer new ways to fight cancer and keep you safe during treatment.
Other New Therapies
Emerging Biologics: A New Hope for Metastatic Cancers includes many new therapies. You see immune checkpoint inhibitors like PD-1 and PD-L1 blockers. New drugs target TIM3, LAG3, TIGIT, and VISTA. Eftilagimod alpha shows promise in lung and breast cancer. Tiragolumab targets TIGIT and helps patients with lung cancer.
Antibody-drug conjugates like ado-trastuzumab emtansine extend survival in HER2-positive breast cancer. Selpercatinib treats lung cancer with RET fusions and works well for brain metastases. Oncolytic viruses attack cancer cells directly. LOAd703 treats pancreatic cancer. GL‑ONC1 is being studied in early‑phase trials for triple‑negative breast cancer.
Here is a list of targeted therapies and their uses:
Vemurafenib targets BRAF in melanoma.
Osimertinib treats lung cancer with EGFR mutations.
Imatinib fights leukemia by blocking BCR-ABL.
Doctors use these therapies to match your treatment to your cancer's unique features. Personalized medicine gives you more options and better results.
Tip: New biologic therapies bring hope and innovation to cancer care.
Emerging Biologics: A New Hope for Metastatic Cancers shows you how science is moving forward. You see safer, more effective treatments that fit your needs. You can feel hopeful about the future of cancer care.
Cancers Benefiting from Biologics
Breast Cancer
You may know that breast cancer is one of the most common cancers. Biologic therapies have changed how doctors treat advanced cases. If you have PD-L1-positive metastatic triple-negative breast cancer, you may receive atezolizumab or pembrolizumab. These medicines help your immune system fight cancer. Studies show that patients can expect a median progression-free survival of about 2.3 months and a median overall survival of 12.1 months. New targeted therapies, like inavolisib plus fulvestrant and palbociclib, also help patients with PIK3CA mutations live longer without cancer growth.
Ovarian Cancer
Ovarian cancer can be hard to treat, especially when it spreads. Biologic therapies offer new hope. Dendritic cell vaccination, when combined with other treatments, has helped some patients live longer without cancer getting worse. You can see this in the table below:
Treatment Type | Impact on Survival Rates |
|---|---|
Chemotherapy | Short-lived responses |
Dendritic Cell Vaccination | Some early‑phase studies show longer progression‑free survival (36–44 months) when dendritic cell vaccines are combined with other treatments, but this approach is still experimental. |
Overall Survival | Modest improvement; over 50% die within five years |
Lung Cancer
Lung cancer is another area where biologics make a big difference. If you have non-small cell lung cancer, you may benefit from immunotherapies like pembrolizumab. Selpercatinib works well for patients with RET fusions, even when cancer spreads to the brain. Selpercatinib shows high response rates (around 64–85%) in patients with RET‑fusion lung cancer, including those with brain metastases. Doctors also use oncolytic viruses and other new treatments to help patients with advanced disease.
Melanoma
Melanoma is a serious skin cancer. Biologic therapies give you more options. Immunotherapies such as PD-1 inhibitors and BRAF inhibitors help your immune system target cancer cells. Amtagvi, a new T cell therapy, shows an objective response rate of 31.5%. Pembrolizumab also brings promising results for patients with advanced melanoma.
Blood Cancers
If you have a blood cancer like leukemia or lymphoma, biologic therapies can change your outlook. CAR T-cell therapy has transformed treatment for some patients, especially those with B-ALL. These therapies target cancer cells and spare healthy ones. Researchers are working on new options, such as bispecific antibodies, oncolytic viruses, and cancer vaccines. These advances help you fight cancer more effectively and with fewer side effects.
You can see that Emerging Biologics: A New Hope for Metastatic Cancers brings real progress for many types of cancer. Each new therapy gives you and your family more reasons to hope.
Effectiveness and Safety
Current Results
You may want to know how well these new treatments work. Clinical trials show that emerging biologics can help many patients with metastatic cancers. Doctors measure effectiveness using numbers like objective response rate (ORR), disease control rate (DCR), median duration of response (mDOR), and median overall survival (mOS). Here is a table that shows recent results for several therapies:
Therapy | ORR (%) | DCR (%) | mDOR (months) | mOS (months) |
|---|---|---|---|---|
Enfortumab vedotin | 23.9 | 56.5 | 9.4 | 6.0 |
Sacituzumab govitecan | 16 | 28 | N/A | 9.0 |
Ozuriftamab vedotin | 32 | N/A | N/A | 11.6 |
Petosemtamab | 36-40.4 | N/A | N/A | 11.5-12.5 |
CUE-101 | N/A | N/A | N/A | 24.4 |
You see that some therapies help patients live longer and control cancer growth. Results vary by therapy and cancer type. Emerging Biologics: A New Hope for Metastatic Cancers gives you more options than ever before.
Common Side Effects
You may worry about side effects. Biologic therapies can cause problems, but most are mild or moderate. Some side effects affect almost any organ in your body. Here are common issues:
Skin problems like rashes
High blood pressure
Low magnesium levels
Heart issues
Most patients tolerate these treatments well. Some may develop serious health problems, so doctors monitor you closely. Here is a table showing side effects and tolerability:
Therapy Type | Side Effects Severity | Tolerability |
|---|---|---|
Conventional Chemotherapy | High | Low |
Immunotherapy (Vaccination) | Mild | High |
Immune Checkpoint Inhibitors | Moderate | Moderate |
Tip: Always tell your care team about any new symptoms. Early action helps prevent serious problems.
Who May Benefit
You may wonder if these therapies are right for you. Doctors find that patients with strong immune responses benefit most. Research shows that people of African ancestry may respond well because their tumors have more immune cells. These therapies can help reduce health disparities. You also benefit if you have specific cancer markers or mutations. Your doctor will help decide which biologic fits your needs.
Note: Personalized medicine means your treatment matches your cancer and your body.
What This Means for Patients
Practical Implications
Emerging biologic therapies change your daily life in many ways. You receive treatments that target cancer cells more precisely. This approach can improve your quality of life and help you feel stronger during treatment. You may notice fewer side effects compared to older therapies. Your immune system gets support to fight cancer, which can make daily activities easier.
Here are some ways these advances affect you and your family:
You get personalized treatment options that fit your cancer type.
Your immune system works better to find and destroy cancer cells.
You may experience improved outcomes and a higher quality of life.
You face challenges like differences in how your body responds to treatment.
Tumor biology can affect how well the therapy works for you.
You need to understand the treatment process. Managing side effects takes patience and teamwork with your healthcare providers. Open communication helps you address fears and expectations. Emotional and practical challenges are common for you and your support system. Participation in clinical trials may offer you improved outcomes.
Tip: Keep track of your symptoms and share them with your care team. This helps you stay safe and get the best results.
Hope and Expectations
You may feel hopeful when starting biologic therapies. Many patients value both quality of life and length of life. Some prefer quality of life, which can reduce cancer-related distress. Your preferences matter when you talk with your doctor. Understanding what you want helps your care team support you better.
Emerging Biologics: A New Hope for Metastatic Cancers gives you new reasons to hope. You see progress in cancer care and more options for treatment. You can expect honest conversations with your healthcare team about what these therapies can do. You may face challenges, but you also gain hope for a better future.
Note: Your journey is unique. Stay informed and ask questions. Your care team wants to help you find the best path forward.
Emerging biologics give you new hope in the fight against metastatic cancers. You see more personalized treatments and better outcomes. Some challenges remain, such as:
Limited effectiveness for some patients
Tumor cells can resist or hide from therapies
Differences in how each person responds
You should talk with your healthcare team about your cancer type, where it has spread, your treatment history, and your health. Stay hopeful. New advances continue to bring better options for you and your loved ones.
FAQ
What makes biologics different from chemotherapy?
Biologics target cancer cells or boost your immune system. Chemotherapy attacks both healthy and cancer cells. Many people experience different or sometimes fewer side effects with biologics compared to chemotherapy.
Can you get biologic therapy for any type of cancer?
You may not get biologics for every cancer. Doctors use them for certain cancers like breast, lung, and blood cancers. Your doctor will decide if they fit your case.
Are biologic therapies safe?
Most people tolerate biologics well. You may have mild side effects like rashes or tiredness. Your care team will watch you closely for any problems.
How do you know if a biologic will work for you?
Doctors test your cancer for special markers. These tests help them choose the best biologic for you. You may need more than one test.
Will insurance cover biologic treatments?
Many insurance plans cover biologics. You should check with your provider. Your care team can help you understand your options.
This article is for educational purposes only and is not a substitute for professional medical advice. For more details, please see our Disclaimer. To understand how we create and review our content, please see our Editorial Policy.
See Also
Key Characteristics and Insights Into Hemangioblastoma
Essential Features and Insights About Glioblastoma
A Simple Overview of Hepatosplenic T-Cell Lymphoma
Simplifying B-Cell Prolymphocytic Leukemia for Better Understanding

