Major Legislative Wins for Cancer Patients in 2025
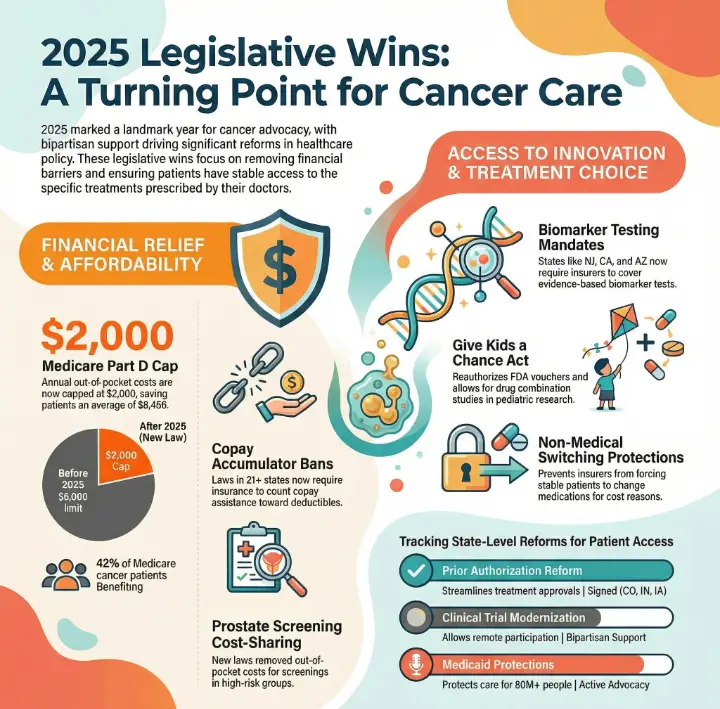
Cancer patients received new hope in 2025 through major legislative wins. Lawmakers approved measures that expanded telehealth flexibilities and boosted pediatric cancer research, as shown below:
Legislative Win | Description |
|---|---|
Telehealth Flexibilities | Temporary extension of Medicare telehealth flexibilities until March 31, 2025 |
Pediatric Cancer Research | Legislation aimed at improving pediatric cancer research |
New laws removed cost-sharing for prostate cancer screenings for high-risk groups and ensured that third-party copay assistance counts toward out-of-pocket limits. Advocacy organizations united communities, raised awareness, and shared patient stories with lawmakers. Their work helped secure these victories. Legislation and Cancer: Recent Wins in Patient Advocacy now reflect the power of collective action and determination.
Key Takeaways
In 2025, new laws improved access to cancer care and reduced costs for patients.
Telehealth flexibilities were extended, allowing more patients to receive care remotely.
States banned copay accumulator programs, ensuring all copay assistance counts toward out-of-pocket costs.
The $2,000 cap on Medicare Part D out-of-pocket expenses significantly lowers costs for cancer patients.
Bipartisan advocacy led to important reforms, showing the power of collective action in healthcare.
Legislation and Cancer: Recent Wins in Patient Advocacy
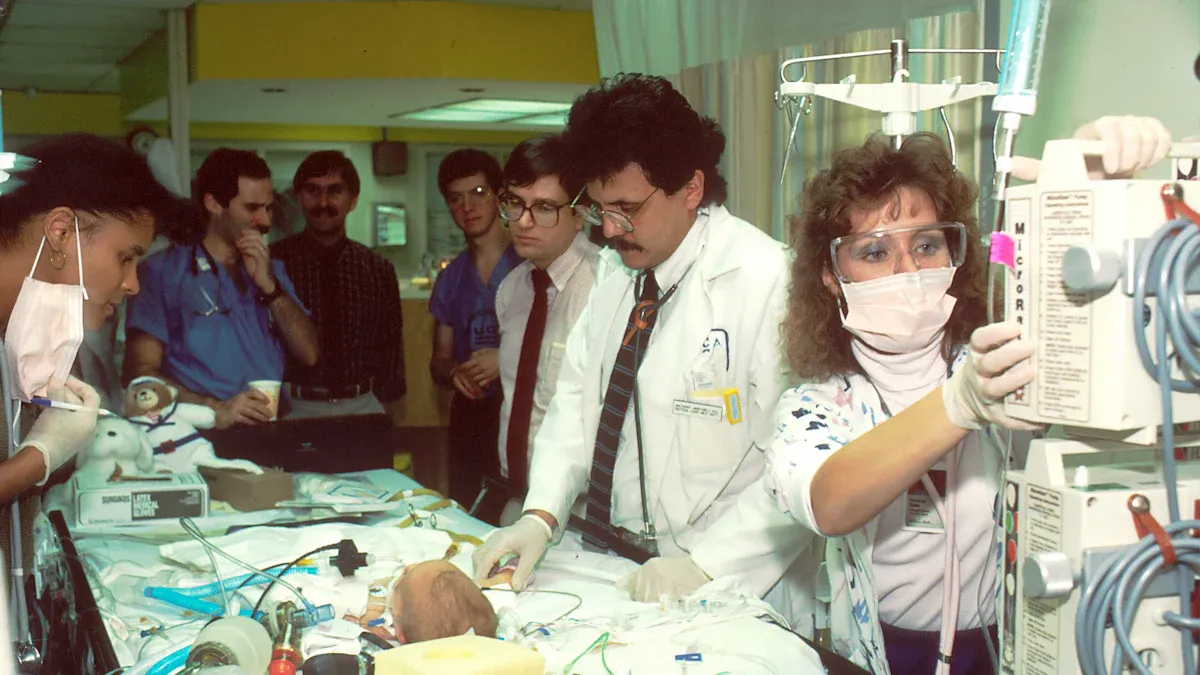
The year 2025 marked a turning point for cancer patients across the United States. Lawmakers passed several new laws that improved access to care, reduced costs, and protected treatment choices. Advocacy groups worked with both political parties to push for these changes. Their efforts led to a wave of reforms that addressed the most pressing needs of cancer patients.
Many states took action to reform insurance practices and protect patients. These changes made it easier for people to get the care they need without unnecessary delays or financial barriers.
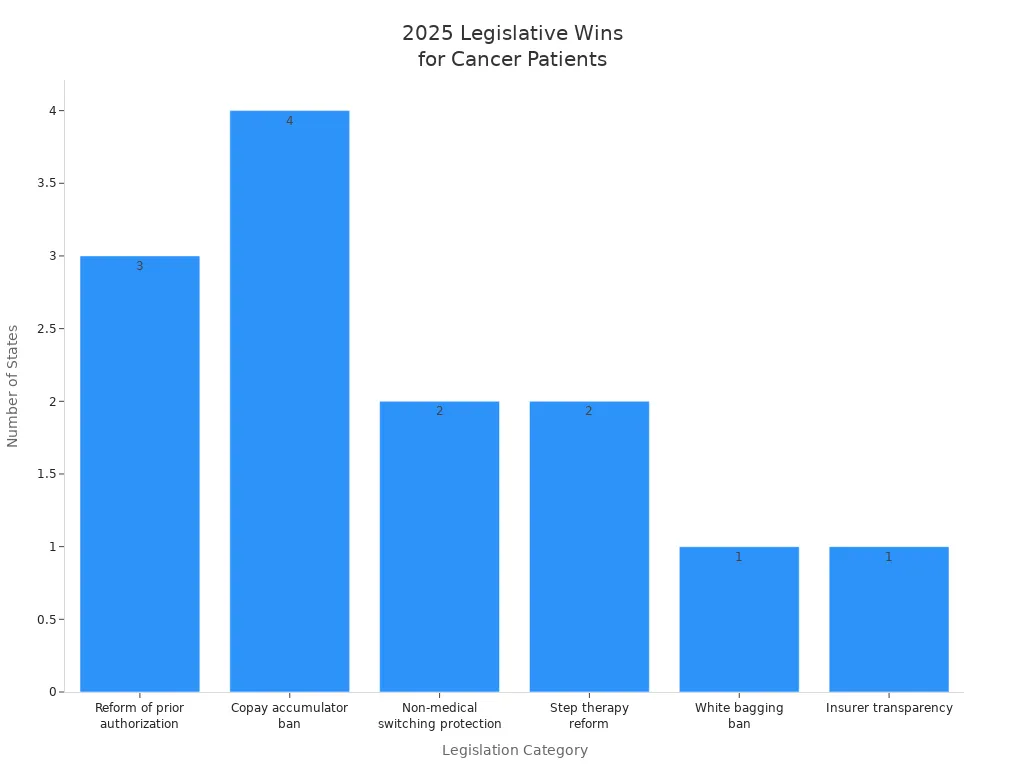
The following table shows the landscape of legislative wins for cancer patients in 2025:
State | Legislation Description | Status |
|---|---|---|
Colorado | Reform of prior authorization practices | Signed into law |
Indiana | Reform of prior authorization practices | Signed into law |
Iowa | Reform of prior authorization practices | Signed into law |
Louisiana | Suspension of prior authorization in Medicaid during emergencies | Signed into law |
Oregon | Enhanced reporting and transparency requirements from insurers | Signed into law |
Alaska | Step therapy bill awaiting governor’s signature | Awaiting signature |
Indiana | Legislation banning copay accumulator programs | Signed into law |
Iowa | Legislation banning copay accumulator programs | Signed into law |
Maryland | Legislation banning copay accumulator programs | Signed into law |
North Dakota | Legislation banning copay accumulator programs | Signed into law |
Arizona | Protection against non-medical switching | Signed into law |
Minnesota | Protection against non-medical switching | Signed into law |
Mississippi | Legislation banning payer-mandated white bagging | Signed into law |
Maine | Step therapy reform for metastatic cancer treatment | Signed into law |
Bipartisan efforts played a key role in passing important laws. The Clinical Trial Modernization Act and the Protecting Patient Access to Cancer and Complex Therapies Act both received support from lawmakers on both sides. These laws help patients join clinical trials more easily and protect access to life-saving treatments.
Legislation Name | Description |
|---|---|
Clinical Trial Modernization Act | Expands trial availability, allows remote participation, and offsets patient burdens. |
Protecting Patient Access to Cancer and Complex Therapies Act | Maintains access to life-saving treatments while balancing drug prices for patients. |
Biomarker Testing Access
Biomarker testing helps doctors choose the best treatment for each patient. In 2025, several states passed laws to make sure insurance covers these important tests. States like New Jersey, California, Illinois, and Arizona led the way. These laws require insurers to pay for biomarker testing when medical evidence supports it.
Key Provision | Description |
|---|---|
Coverage Mandates | Laws require insurers to cover biomarker testing when supported by medical evidence. |
Legislative Actions | States like New Jersey, California, Illinois, and Arizona are expanding access. |
Addressing Disparities | Efforts ensure fair access to biomarker testing for all groups and regions. |
Policy Recommendations | Suggestions include comprehensive coverage and more testing in underserved areas. |
These changes help reduce disparities and give more patients a chance at better outcomes.
Copay Accumulator Ban Laws
Many cancer patients rely on copay assistance to afford their medicines. In 2025, more states banned copay accumulator programs. These programs had stopped copay help from counting toward a patient’s out-of-pocket costs. Now, laws require health plans and pharmacy benefit managers to count all copay assistance toward deductibles and out-of-pocket maximums.
Feature | Description |
|---|---|
Requirement for Health Plans and PBMs | Must count all forms of copay assistance toward a patient’s deductible and out-of-pocket maximum. |
Ban on Accumulator Programs | Bans programs that exclude copay assistance from cost-sharing calculations. |
State-Level Actions | 21 states have enacted laws prohibiting these programs for state-regulated plans. |
At least 16.8% of the US commercial market, or about 34.28 million people, now benefit from these protections.
Since 2019, 25 states, DC, and Puerto Rico have banned copay accumulator programs.
These laws make cancer treatment more affordable for many families.
Non-Medical Switching Protections
Non-medical switching happens when insurance companies make patients change medicines for reasons not related to health. In 2025, Arizona and Minnesota passed laws to stop this practice. These laws protect patients from being forced to switch medications during the plan year if their doctor says it is not safe.
Continuity of care is important for patients who are stable on their medicines.
Changes to drug lists should happen before the plan year starts so patients can make informed choices.
Doctors should have the power to keep patients on the best treatment.
"Our study suggests a negative impact on patient care during the reform’s implementation period, representing a survival risk. It is essential to ensure adequate monitoring and support to prevent adverse effects on patients’ health."
Non-medical switching can disrupt cancer treatment and put patients at risk. These new protections help patients stay on the therapies that work best for them.
Legislation and Cancer: Recent Wins in Patient Advocacy show how strong advocacy and bipartisan teamwork can lead to real change. Patients, families, and providers now have more tools and protections than ever before.
Improving Access and Affordability

Medicare Part D $2,000 Cap
Medicare beneficiaries with cancer often face high costs for prescription drugs. In 2025, a new $2,000 annual cap on out-of-pocket expenses for Medicare Part D prescription medications took effect. This cap includes deductibles, copayments, and coinsurance for all covered drugs. Specialty medications, which can be very expensive, are also included. The cap does not apply to drugs outside Part D or to monthly premiums. Before this change, patients could pay up to $8,000 each year. Now, the maximum is $2,000. This reform is part of the Inflation Reduction Act. It applies to all Medicare beneficiaries with Part D coverage. About 42% of Medicare Part D beneficiaries with cancer will benefit. These patients are expected to save an average of $8,486 each year.
Many cancer patients now have better access to life-saving medicines without facing overwhelming costs.
Early Screening Legislation
Early detection saves lives. In 2025, Congress passed the SCREENS for Cancer Act. This law supports the National Breast and Cervical Cancer Early Detection Program. The program helps more people get screened for cancer at an early stage. Studies show that cancer screening recommendations can lower deaths from cancers like cervical and colorectal cancer. The impact of early detection depends on the type of cancer and the population. Screening can also have risks, such as overdiagnosis. Lawmakers continue to review and improve these programs to maximize benefits and reduce harm.
Legislation Name | Year Introduced | Purpose | Programs Supported |
|---|---|---|---|
SCREENS for Cancer Act | 2025 | Improve cancer detection | National Breast and Cervical Cancer Early Detection |
Medicaid and Marketplace Updates
Medicaid and Marketplace plans help many cancer patients afford care. In 2025, several changes affected these programs. Some states added work requirements for Medicaid enrollment. These rules may cause people to lose coverage, making it harder to get cancer treatment. Cost-sharing increased for low-income Medicaid enrollees, raising the financial burden for families. Frequent eligibility checks and reduced retroactive eligibility put patients at risk of losing coverage and facing medical debt. Changes to Marketplace plans, such as ending autoenrollment and eliminating caps on tax credit repayment, add stress and administrative hurdles.
Change Description | Impact on Cancer Patients |
|---|---|
Work requirements for Medicaid enrollment | Many may lose coverage, complicating access to cancer care |
Cost-sharing for low-income enrollees | Increased financial burden for cancer-related care |
Frequent eligibility redetermination | Higher risk of losing coverage, affecting continuity of care |
Reduced retroactive eligibility | More medical debt, possible hospital closures |
Blocking access to Marketplace plans | Loss of tax credits, less affordable coverage |
Ending autoenrollment in Marketplace plans | Risk of losing coverage due to administrative burden |
Eliminating cap on tax credit repayment | Potential for significant tax liabilities |
Legislation and Cancer: Recent Wins in Patient Advocacy highlights how new laws can both help and challenge patients. Ongoing advocacy remains essential to protect access and affordability for everyone facing cancer.
Safeguarding Patient Treatment Choices
Protecting Patient Access to Cancer and Complex Therapies Act
The Protecting Patient Access to Cancer and Complex Therapies Act became a key law in 2025. Lawmakers designed this act to protect Medicare patients from losing access to important treatments. The act addresses payment cuts under Medicare Part B and ensures that patients can continue to receive advanced therapies. A strong coalition of patient groups and healthcare providers supported this law. Bipartisan support helped move the legislation forward.
Provision | Description |
|---|---|
Purpose | To protect Medicare beneficiaries’ access to care and address Medicare Part B payment cuts. |
Coalition | Endorsed by the Part B Access to Seniors and Physicians Coalition. |
Legislation | Bipartisan support for H.R. 4299, aimed at improving patient access to cancer and complex therapies. |
This law gives patients more stability and helps doctors provide the best care.
Pediatric Cancer Trial Access (Give Kids a Chance Act)
Children with cancer need access to new treatments. The Give Kids a Chance Act made it easier for researchers to study new drugs for children. The law requires timely pediatric studies and expands programs that reward companies for developing new treatments. It also allows researchers to test combinations of drugs, which can lead to better results for young patients.
Provision | Description |
|---|---|
Timely Pediatric Studies | Ensures that pediatric studies for new treatments are completed on time by improving existing laws. |
Reauthorization of FDA Priority Review Voucher Program | Expands the program to incentivize pediatric research, reauthorizing it until 2029. |
Combination Studies | Allows researchers to study combinations of new cancer drugs, potentially leading to new treatments for children. |
This act brings hope to families and encourages innovation in pediatric cancer care.
State Advocacy Highlights
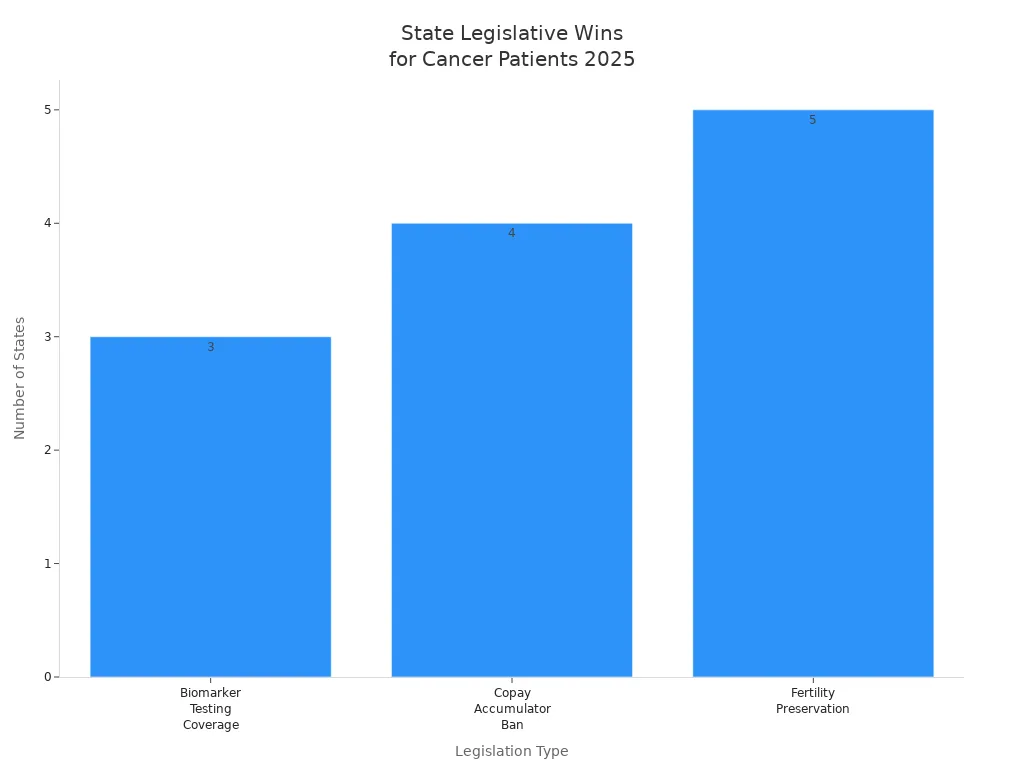
State-level advocacy led to many wins for cancer patients in 2025. States passed laws to cover biomarker testing, ban copay accumulator programs, and require fertility preservation coverage for cancer patients. These changes help patients get the care they need.
In 2025, Ernie Davis, a senior director at the Leukemia & Lymphoma Society, established strong relationships with lawmakers, leading to the passage of laws in seven states that protect patients from harmful medical debt.
Approximately 350 advocates from 40 states met with 222 members of Congress to push for better cancer treatments.
ASCO worked with healthcare organizations to prevent Medicaid cuts, protecting access to care for over 80 million Americans. These efforts show the power of advocacy in improving patient outcomes.
Lawmakers made measurable progress for cancer patients in 2025:
Measure Type | Description | Status |
|---|---|---|
Prior Authorization Reform | Streamlines approvals for cancer treatments | Awaiting Governor's Signature |
Co-Pay Accumulator Reform | Improves patient access to treatments | Awaiting Governor's Signature |
Breast Cancer Screening Access | Expands access to additional screenings | Passed Senate |
Patients now benefit from better care quality, lower costs, and improved access. The ROCR Act 2025 introduced episode-based payments and transportation help for underserved groups. Advocacy groups continue to push for tobacco control, stronger screening programs, and financial relief. Experts expect value-based care, new drug options, and state innovation to empower patients even more. Ongoing advocacy will shape a brighter future for everyone facing cancer.
FAQ
What is a copay accumulator program?
A copay accumulator program stops copay assistance from counting toward a patient’s deductible or out-of-pocket maximum. Many states banned these programs in 2025. Patients now see all copay help count toward their costs.
How does the Medicare Part D $2,000 cap help cancer patients?
The $2,000 cap limits annual out-of-pocket costs for prescription drugs. Cancer patients with Medicare Part D save money on expensive medicines. This change makes treatment more affordable.
Who benefits from biomarker testing laws?
Patients with cancer
Doctors who need precise information
Families seeking better outcomes
These laws require insurance to cover important tests. More patients receive personalized treatment.
What protections exist against non-medical switching?
A new law in 2025 prevents insurers from forcing patients to change medicines for non-medical reasons. Doctors decide if a patient should stay on a current drug. This protects treatment plans.
This article is for educational purposes only and is not a substitute for professional medical advice. For more details, please see our Disclaimer. To understand how we create and review our content, please see our Editorial Policy.
See Also
Exploring Cancer Types Associated With AIDS Infection
An In-Depth Overview of Various Cancer Categories
Insights Into Lymphoma Associated With AIDS
A Deep Dive Into Large-Cell Lung Cancer Classification
Recognizing Symptoms and Treatment Options for Conjunctival Melanoma

