Understanding Malignant Fibrous Histiocytoma of Bone and Osteosarcoma
Malignant fibrous histiocytoma of bone/osteosarcoma are rare yet highly aggressive forms of bone cancer. These diseases predominantly affect individuals aged 10 to 30 years and represent approximately 2% of all childhood cancers, with an even smaller occurrence in adults. Early detection is crucial for improving patient outcomes, as malignant fibrous histiocytoma of bone/osteosarcoma respond similarly to chemotherapy, achieving a 5-year metastasis-free survival rate of around 61%. Despite progress in treatment options, these cancers continue to have a profound impact on patients' quality of life, underscoring the importance of prompt diagnosis and intervention.
Statistic | Value |
|---|---|
New cases diagnosed annually | About 1,000 in the U.S. |
Age group most affected | 10 to 30 years old |
Percentage of childhood cancers | |
Percentage of adult cancers | Much smaller than childhood |
Key Takeaways
Malignant fibrous histiocytoma and osteosarcoma are serious bone cancers. They mostly affect people aged 10 to 30. Finding them early helps improve survival chances.
Symptoms include constant bone pain, swelling, and trouble moving. Spotting these signs early can lead to faster treatment.
Surgery is the main way to treat these cancers. It is often paired with chemotherapy to work better. Doctors try to save as much healthy tissue as possible.
Genetic traits and things like radiation exposure can raise cancer risks. Living a healthy life might lower the chances of getting these cancers.
New treatments like immunotherapy and targeted therapy look promising. Learning about these new options gives hope for better results.
What Are Malignant Fibrous Histiocytoma of Bone and Osteosarcoma?
Malignant Fibrous Histiocytoma of Bone
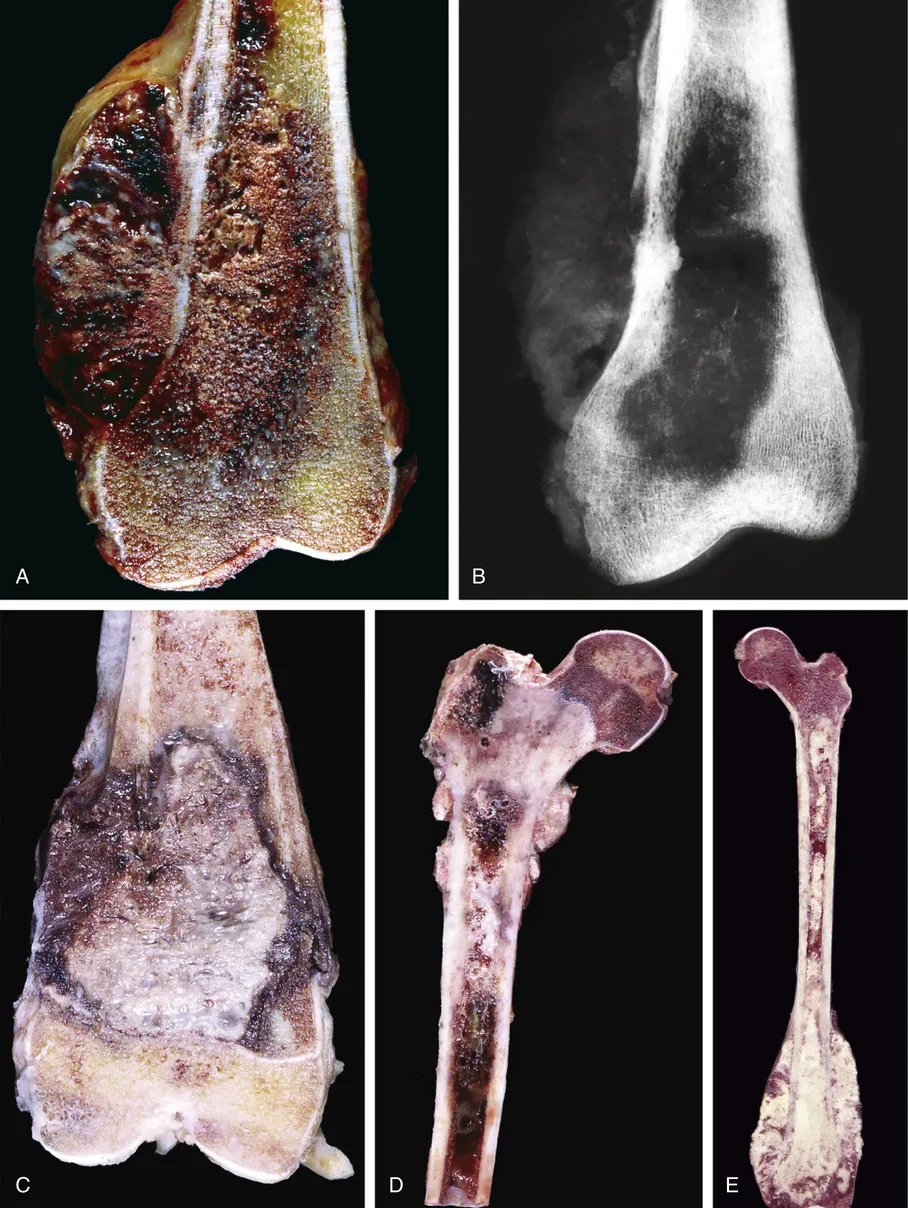
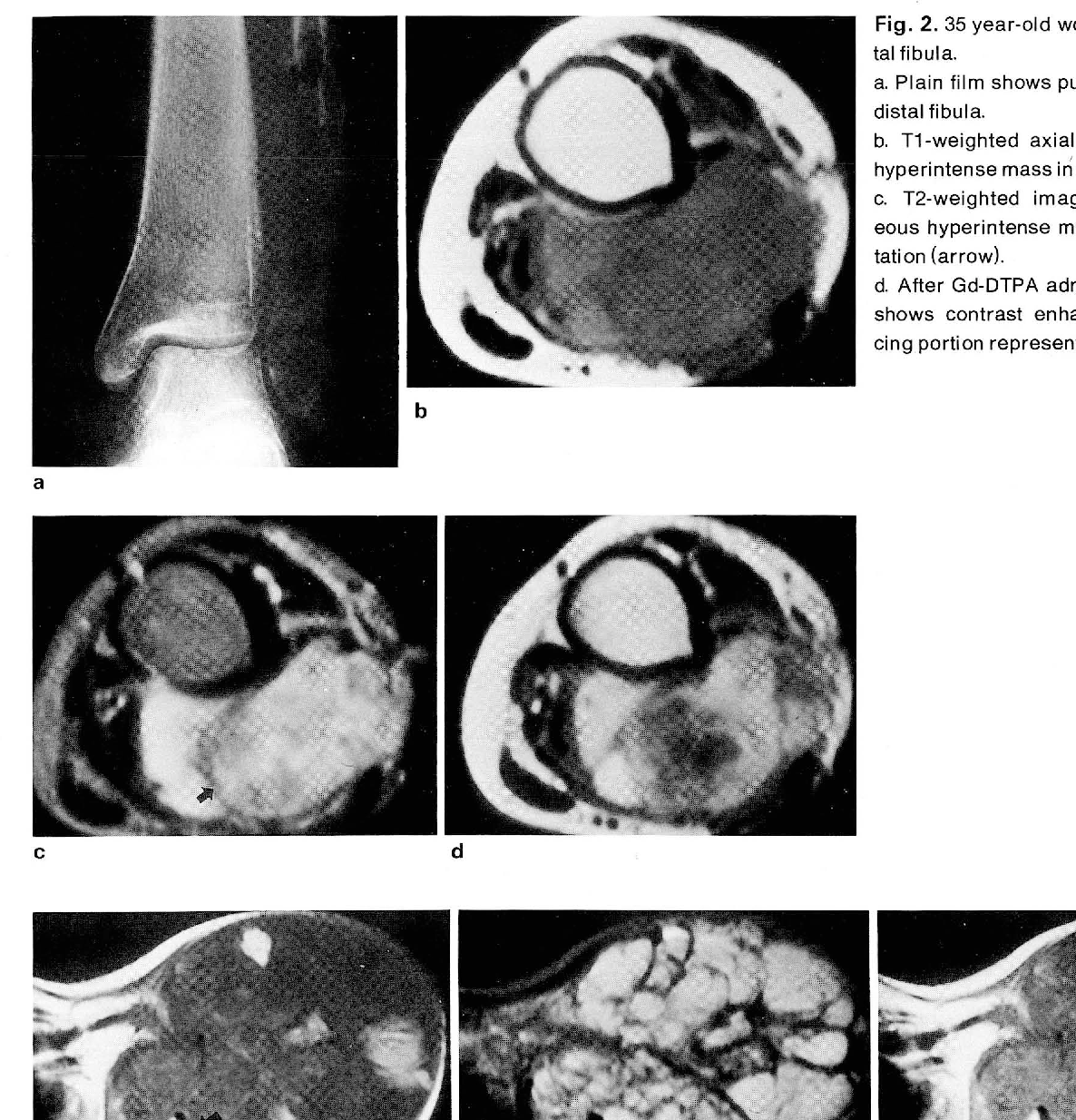
Malignant fibrous histiocytoma of bone is a rare, high-grade sarcoma that primarily affects older adults. It is characterized by a pleomorphic and bimodal pathology, with collagen production serving as a key differentiating feature. Imaging techniques such as CT and MRI often reveal mixed-density signals, internal hemorrhage, and lobular growth patterns. Bone scans typically show increased uptake in the adjacent cortex. Histologically, this cancer exhibits a storiform pattern of fibrous tissue, large foamy histiocytes, and atypical cells with necrosis and vascular invasion. Grossly, the tumor may display a lobular growth pattern with a reactive capsule and varying fat content.
Osteosarcoma
Osteosarcoma originates from malignant mesenchymal cells that differentiate into osteoblasts. It commonly arises in the metaphyses of long bones, such as the distal femur, proximal tibia, and proximal humerus, particularly during adolescence when bone growth is most active. This cancer is defined by the presence of malignant osteoid tissue and cartilage. Conventional central osteosarcoma, the most common subtype, often shows areas of necrosis and atypical mitoses. Osteosarcoma can metastasize to the lungs or other bones, forming "skip lesions."
Differences Between Malignant Fibrous Histiocytoma of Bone and Osteosarcoma
Although malignant fibrous histiocytoma of bone and osteosarcoma share similarities, they differ in several key aspects. Osteosarcoma typically affects younger patients and presents with larger tumor volumes, while malignant fibrous histiocytoma of bone is more common in older individuals and often exhibits an osteolytic pattern. Chemosensitivity is higher in osteosarcoma, whereas some patients with malignant fibrous histiocytoma of bone respond well to radiation therapy. Both cancers have comparable survival rates and prognoses, though osteosarcoma is generally considered more radioresistant.
Causes and Risk Factors
Genetic Causes
Genetic mutations play a significant role in the development of malignant fibrous histiocytoma of bone/osteosarcoma. Several key mutations have been identified:
Mutations in the p53 tumor suppressor gene, which regulates cell division and prevents tumor formation.
Alterations in the RB1 tumor suppressor gene, commonly associated with retinoblastoma but also linked to bone cancers.
Chromosomal abnormalities, particularly gains in the 22q region, which includes the PDGF-B gene involved in cell growth and division.
These genetic changes disrupt normal cellular processes, leading to uncontrolled growth and the formation of malignant tumors.
Environmental and Lifestyle Factors
While genetic predisposition is critical, environmental and lifestyle factors may also contribute to the risk of developing these cancers. Exposure to ionizing radiation, either through medical treatments or environmental sources, has been linked to an increased likelihood of bone sarcomas. Additionally, individuals with a history of Paget’s disease, a condition that weakens bones, face a higher risk. Lifestyle factors, such as smoking and poor dietary habits, may indirectly influence cancer risk by weakening the immune system and overall bone health.
Age, Gender, and Other Risk Factors
Age and gender significantly influence the risk of developing malignant fibrous histiocytoma of bone/osteosarcoma.
Osteosarcoma most commonly affects individuals aged 10 to 30, particularly during teenage growth spurts. Males are more frequently diagnosed than females, although females may develop it earlier due to earlier growth spurts.
Malignant fibrous histiocytoma of bone is more prevalent in individuals over 50. It is slightly more common in males than females.
Other risk factors include a history of bone trauma or chronic bone conditions. These factors, combined with genetic and environmental influences, create a complex risk profile for these aggressive cancers.
Symptoms and Diagnosis
Symptoms of Malignant Fibrous Histiocytoma of Bone
Malignant fibrous histiocytoma of bone presents with a range of symptoms that often worsen over time. These include:
Symptom | Description |
|---|---|
Pain | Commonly occurs, especially when the tumor is near nerves; can be dull or sharp. |
Swelling | Enlargement of the affected area, may be firm or soft, often with redness or warmth. |
Limited range of motion | Can cause stiffness and reduced mobility in affected joints. |
Fractures | Weakened bones increase the risk of fractures or breaks. |
Fatigue | May lead to weakness and tiredness, especially if the tumor has spread. |
Weight loss | Can occur alongside loss of appetite and general malaise. |
These symptoms often mimic other conditions, making early diagnosis critical for effective treatment.
Symptoms of Osteosarcoma
Osteosarcoma symptoms often overlap with other bone conditions, but certain signs are more indicative of this cancer:
Swelling over a bone or bony part of the body.
Pain in a bone or joint, which may worsen at night or during activity.
A bone that breaks for no known reason.
Localized tenderness and decreased range of motion are also common. Some patients experience soft tissue swelling or unexplained fevers, which can complicate diagnosis.
Diagnostic Methods
Imaging Techniques
Accurate imaging is essential for diagnosing malignant fibrous histiocytoma of bone/osteosarcoma. The following techniques are commonly used:
Imaging Technique | Description |
|---|---|
X-ray | Uses energy beams to create images of bones and organs, helping visualize tumor location. |
CT scan | Produces detailed body images from different angles, often with dye, to assess tumor extent. |
MRI | Employs magnets and radio waves to generate detailed images, revealing soft tissue involvement. |
These methods provide critical insights into tumor size, location, and potential metastasis.
Biopsy Procedures
A biopsy remains the definitive method for diagnosing bone cancers. Key steps include:
A surgeon removes cells or tissues for microscopic examination.
The procedure must align with the surgical plan to ensure effective treatment.
Types of biopsies include core biopsy (using a wide needle) and incisional biopsy (removing part of a lump).
Step | Description |
|---|---|
1 | Confirms the diagnosis of bone cancer and establishes tumor grade. |
2 | Conducted by an experienced surgeon to minimize risks of contamination and misdiagnosis. |
3 | Careful planning ensures complete removal of malignant cells and facilitates limb salvage. |
Proper coordination between diagnostic and treatment teams is vital for successful outcomes.
Treatment Options
Surgery
Surgery remains the cornerstone of treatment for malignant fibrous histiocytoma of bone/osteosarcoma. Surgeons aim to remove the tumor entirely while preserving as much healthy tissue as possible. Limb-salvage surgery is often preferred over amputation, with success rates reaching 92% for malignant fibrous histiocytoma of bone and 85% for osteosarcoma. Disease-free survival rates are also comparable, standing at 67% and 65%, respectively.
Condition | Limb Salvage Rate | Disease-Free Survival Rate |
|---|---|---|
MFH of Bone | 92% | 67% |
Osteosarcoma | 85% | 65% |
The prognosis for both conditions is similar, with surgical outcomes significantly improving when combined with other treatments. Proper surgical planning ensures complete tumor removal, reducing the risk of recurrence.
Chemotherapy
Chemotherapy plays a critical role in managing osteosarcoma and, to a lesser extent, malignant fibrous histiocytoma of bone. It is typically administered before surgery to shrink tumors and afterward to eliminate residual cancer cells. Commonly used drugs include:
Methotrexate (administered in high doses with leucovorin to mitigate side effects)
Doxorubicin
Cisplatin or carboplatin
Ifosfamide
Cyclophosphamide
Etoposide
Gemcitabine
This approach reduces the likelihood of cancer recurrence and improves long-term survival rates. Chemotherapy is particularly effective in osteosarcoma cases, where it enhances the success of surgical interventions.
Radiation Therapy
Radiation therapy is less commonly used for osteosarcoma due to its radioresistant nature but remains valuable in specific scenarios. It helps manage pain and is often employed when surgical margins are inadequate, especially in head and neck osteosarcoma. For malignant fibrous histiocytoma of bone, radiation therapy can improve local control rates, particularly in cases with positive or uncertain resection margins. It is also used to treat recurrent osteosarcoma in different bones, offering an alternative when surgery is not feasible.
Radiation therapy provides a non-invasive option for patients with limited surgical options, enhancing their quality of life and controlling disease progression.
Emerging Therapies
The field of oncology continues to evolve, offering hope through innovative therapies for malignant fibrous histiocytoma of bone and osteosarcoma. Emerging treatments aim to improve survival rates and reduce side effects associated with traditional methods.
Immunotherapy
Immunotherapy harnesses the body’s immune system to combat cancer. Researchers are exploring immune checkpoint inhibitors, such as PD-1/PD-L1 blockers, to enhance the immune response against tumor cells. Early trials have shown promise in improving outcomes for patients with advanced or recurrent osteosarcoma. Additionally, CAR-T cell therapy, which modifies a patient’s T-cells to target specific cancer antigens, is under investigation for its potential to deliver personalized treatment.
Note: Immunotherapy represents a significant shift in cancer treatment, focusing on the body’s natural defenses rather than directly targeting the tumor.
Targeted Therapy
Targeted therapies focus on specific molecules involved in cancer growth. Drugs like tyrosine kinase inhibitors (TKIs), including cabozantinib and regorafenib, have demonstrated efficacy in slowing tumor progression. These therapies minimize damage to healthy tissues, offering a more precise approach compared to chemotherapy. Ongoing studies aim to identify additional molecular targets to expand treatment options.
Experimental Approaches
Several experimental therapies are in development, including gene therapy and nanotechnology-based drug delivery systems. Gene therapy seeks to correct genetic mutations responsible for cancer, while nanotechnology enhances drug delivery to tumors, improving efficacy and reducing toxicity. Clinical trials are critical in evaluating these cutting-edge techniques.
Therapy Type | Example Treatments | Current Status |
|---|---|---|
Immunotherapy | PD-1 inhibitors, CAR-T cells | Early clinical trials |
Targeted Therapy | Cabozantinib, Regorafenib | FDA-approved for trials |
Experimental Methods | Gene therapy, Nanotechnology | Preclinical/Phase I |
Emerging therapies offer new avenues for treating these aggressive cancers. Continued research and clinical trials remain essential to bring these advancements to patients worldwide.
Prevention and Prognosis
Prevention Strategies
Preventing malignant fibrous histiocytoma of bone/osteosarcoma remains challenging due to its complex etiology. While genetic predispositions cannot be altered, certain strategies may reduce risk:
Avoiding unnecessary exposure to ionizing radiation, especially during childhood.
Maintaining a healthy lifestyle to support overall bone health, including a balanced diet rich in calcium and vitamin D.
Regular medical check-ups for individuals with a family history of bone cancers or genetic syndromes like Li-Fraumeni syndrome.
Public awareness campaigns can also play a role in educating communities about early symptoms, encouraging timely medical evaluations.
Prognosis for Malignant Fibrous Histiocytoma of Bone and Osteosarcoma
Several factors influence the prognosis for patients diagnosed with these aggressive bone cancers:
The type of surgical margins achieved during tumor removal. Wide or radical margins significantly improve outcomes.
The primary tumor site and its size. Tumors in accessible locations are easier to treat.
The presence of metastatic disease at diagnosis. Patients without metastases have better survival rates.
The degree of tumor necrosis following neoadjuvant chemotherapy. Higher necrosis rates correlate with improved outcomes.
Patient demographics, including age and sex, also play a role.
Other factors, such as the tumor's resectability and the patient's overall health, further shape the prognosis. Early and aggressive treatment remains critical for improving survival rates.
Importance of Early Diagnosis and Treatment
Early diagnosis of malignant fibrous histiocytoma of bone/osteosarcoma significantly enhances survival rates. These cancers progress rapidly, making timely intervention essential. Delays in diagnosis often occur due to vague symptoms or misinterpretation of initial signs. Recognizing symptoms like persistent bone pain or swelling can prompt earlier imaging and biopsy procedures.
Evidence Type | Description |
|---|---|
Aggressive Nature | Bone cancers are aggressive, making early diagnosis critical for outcomes. |
Diagnostic Delays | Delays worsen prognosis, emphasizing timely intervention. |
Radiography Importance | Prompt radiography reduces diagnostic delays. |
Referral to Cancer Centers | Specialized care maximizes survival and quality of life. |
Patients benefit from expedited referrals to cancer centers, where multidisciplinary teams can provide comprehensive care. Early detection not only improves survival but also enhances the quality of life by enabling less invasive treatments.
Malignant fibrous histiocytoma of bone and osteosarcoma are rare but aggressive cancers that demand early detection and prompt treatment. Raising awareness about symptoms and risk factors can lead to timely medical intervention, improving survival rates. Recent advancements in research and treatment offer hope for better outcomes:
Immunotherapy targeting GD2 shows promise in clinical trials.
Computer-assisted tumor surgery enhances surgical precision.
New internal prostheses benefit growing children by eliminating the need for repeated surgeries.
These innovations highlight the progress being made, inspiring optimism for patients and their families. Continued research will undoubtedly pave the way for more effective therapies.
FAQ
What is the survival rate for osteosarcoma and malignant fibrous histiocytoma of bone?
The 5-year survival rate for localized osteosarcoma is approximately 70%. For malignant fibrous histiocytoma of bone, survival rates are similar when treated early. Prognosis worsens significantly if metastasis occurs, emphasizing the importance of early diagnosis and comprehensive treatment.
Can these cancers be prevented?
Prevention is challenging due to genetic factors. However, reducing exposure to ionizing radiation and maintaining bone health through a balanced diet and regular exercise may lower risks. Individuals with a family history should seek regular medical evaluations to monitor potential early signs.
How are these cancers diagnosed?
Doctors use imaging techniques like X-rays, CT scans, and MRIs to identify tumors. A biopsy confirms the diagnosis by analyzing tissue samples under a microscope. Early and accurate diagnosis is critical for effective treatment planning and improved outcomes.
Are children more at risk for osteosarcoma?
Yes, osteosarcoma primarily affects children and adolescents during growth spurts, particularly those aged 10 to 30. Rapid bone growth during puberty increases susceptibility. Boys are slightly more at risk than girls, though girls may develop it earlier due to earlier growth spurts.
What are the latest advancements in treatment?
Emerging therapies include immunotherapy, such as CAR-T cell therapy, and targeted drugs like tyrosine kinase inhibitors. Experimental approaches, including gene therapy and nanotechnology, show promise in clinical trials. These innovations aim to improve survival rates and reduce treatment side effects.
Note: Patients should consult oncologists to explore the most suitable treatment options based on their specific diagnosis.
See Also
Exploring Fibrocartilaginous Mesenchymoma Found in Bone
Defining Fibrosarcoma: Essential Features and Insights
A Comprehensive Overview of Angiosarcoma

