What Is Precision Medicine and How Does It Work

You experience healthcare differently with precision medicine. This approach uses your genetic makeup, environment, and daily habits to shape your care. Unlike traditional methods, you do not receive a one-size-fits-all treatment.
Precision medicine looks for early signs of disease and can help prevent illness.
You get therapies designed for your body, which can mean faster diagnoses and better results.
Precision Medicine: Tailoring Treatments to Genetic Profiles gives you care that fits your unique needs.
Key Takeaways
Precision medicine tailors treatments to your unique genetic makeup, environment, and lifestyle, leading to better health outcomes.
This approach helps doctors predict how you will respond to therapies, increasing your chances of success and reducing side effects.
Genetic testing plays a crucial role in precision medicine, allowing doctors to choose the safest and most effective medications for you.
Precision medicine shows significant improvements in cancer care, with higher response rates and longer survival times compared to traditional treatments.
Access to precision medicine can be limited by costs and geographic disparities, highlighting the need for equitable healthcare solutions.
Precision Medicine: Tailoring Treatments to Genetic Profiles

What Sets Precision Medicine Apart
You see a big difference when you compare Precision Medicine: Tailoring Treatments to Genetic Profiles with traditional medicine. Precision medicine uses your genetic information, environment, and lifestyle to create a treatment plan just for you. Traditional medicine often gives everyone the same treatment, no matter their unique traits. This shift means you get care that fits your needs.
Here is a table that shows how these two approaches differ:
Aspect | Precision Medicine | Traditional Medicine |
|---|---|---|
Treatment Approach | Tailored to individual genetic, environmental, and lifestyle factors | One-size-fits-all approach |
Effectiveness | Improved effectiveness due to personalized therapies | Variable effectiveness |
Side Effects | Reduced side effects | Higher risk of side effects |
Example in Oncology | Targeted therapies for specific genetic mutations | General chemotherapy or radiation therapy |
You benefit from targeted therapies, especially in cancer care. Doctors can focus on specific genetic mutations in your cancer cells. This leads to treatments that work better and cause fewer side effects than traditional chemotherapy. Precision Medicine: Tailoring Treatments to Genetic Profiles gives you more hope for a positive outcome.
Personalization Through Genetics
Your genes play a key role in how doctors choose your treatments. Precision Medicine: Tailoring Treatments to Genetic Profiles uses biomarkers to predict how you will respond to certain therapies. For example, doctors look for mutations in genes like EGFR or BRAF. If you have these mutations, you may receive targeted therapies that match your genetic profile.
Pharmacogenomics helps doctors understand how your body handles medicine. Your genes can change how you break down drugs. Some people process medicine quickly, while others do it slowly. This difference can affect how well a drug works or if it causes side effects. Doctors use tests to find out if you have gene variants, such as TPMT, that could make some medicines dangerous for you. The FDA recommends genetic testing before giving certain drugs to keep you safe.
The Clinical Pharmacogenetics Implementation Consortium (CPIC) gives doctors guidelines for matching drugs to your genes. This helps you get the right medicine at the right dose. For example, the enzyme CYP2D6 affects how you respond to pain medicine like codeine. If you are a poor metabolizer, you may not feel relief. If you are an ultra-rapid metabolizer, you could have harmful side effects. Knowing your genetic profile helps doctors choose the best treatment for you.
Doctors have seen better results when they use Precision Medicine: Tailoring Treatments to Genetic Profiles. Recent studies show that response rates improve when treatments are genomically matched, but the exact percentage varies by cancer type and trial. These patients also live longer without their disease getting worse. You can see the difference in the chart below:
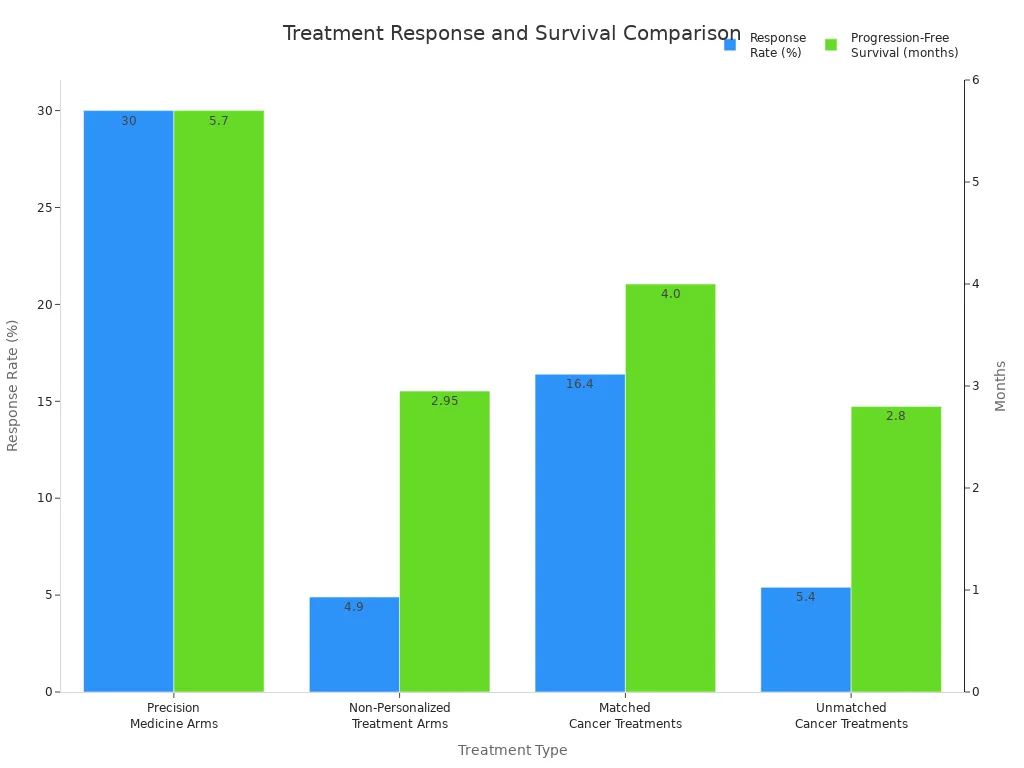
You get a higher chance of success and fewer side effects when your treatment matches your genetic profile. Precision Medicine: Tailoring Treatments to Genetic Profiles gives you a path to safer and more effective care.
How Precision Medicine Works

Genomics and Biomarkers
You play a key role in your own healthcare when you use precision medicine. Doctors gather information about your genes, environment, and lifestyle to create a treatment plan that fits you. This approach uses genomics and biomarkers to guide decisions.
Genomics looks at your DNA to find changes that may cause disease. Biomarkers are signals in your body, like proteins or genetic mutations, that help doctors understand your health. These tools help with:
Diagnosis: Doctors use genomics and biomarkers to find diseases and see how serious they are.
Prognosis: You can learn how your disease might progress with standard treatment.
Treatment Selection: Your doctor can choose the best therapy for you based on your unique profile.
Pharmacogenomic Testing: You find out how your genes affect your response to certain medicines.
Multi-Omics Integration: Doctors combine data from different sources, such as genes, proteins, and metabolism, to get a complete picture of your health.
Doctors use these methods to spot early signs of disease, track how well treatments work, and adjust your care as needed. For example, they can detect treatment resistance before you feel symptoms or see changes on scans. They also monitor your blood for tiny pieces of tumor DNA, called ctDNA, to check if your treatment is working.
You benefit from these advances because they help doctors make better decisions. In some studies, like the NCI-MATCH trial, doctors used biomarker tests to match patients with the right treatments. The table below shows how often these tests led to positive outcomes:
Study Name | Patient Population | Positive Outcome Rate |
|---|---|---|
NCI-MATCH Trial | 6,000 patients with treatment-resistant solid tumors | 25.9% (7 of 27 substudies) |
This means that about one in four patients found a treatment that worked better for them because of biomarker testing.
Data-Driven Decisions
You see the power of data in precision medicine every day. Doctors use large sets of information from many patients to find patterns and make better choices for you. They look at your genetic data, your environment, and your lifestyle to predict your risks and choose the best treatments.
Here is how data-driven decisions help you:
Big data analytics tailors treatments to your unique traits, such as your genes and habits.
Doctors analyze large amounts of genomic and clinical data to find important biomarkers and predict disease risks.
Personalized treatment strategies improve your health and can lower healthcare costs.
Precision medicine aims to give you the right treatment at the right time, making care more effective.
AI-driven data integration brings together information from your medical records, genetic tests, and even wearable devices.
This approach helps doctors spot early warning signs, track your health over time, and adjust your care before problems get worse.
Doctors often work together in groups called multidisciplinary tumor boards (MDTBs). These teams review your genomic data and help decide the best treatment plan. The table below shows how MDTBs impact your care:
Role of MDTBs | Impact on Treatment Decisions |
|---|---|
Interpretation of genomic data | 55.8% of cases saw treatment changes based on MDTB advice |
Validation of clinical decisions | Adds another layer of safety and accuracy |
Medical education | Helps doctors learn and stay up to date |
Collaboration | Brings together experts from different fields |
You benefit from this teamwork because it leads to more accurate and personalized care. Doctors can detect changes in your health earlier and adjust your treatment quickly. With Precision Medicine: Tailoring Treatments to Genetic Profiles, you get care that keeps up with your needs and gives you the best chance for a good outcome.
Benefits of Precision Medicine
Better Outcomes
You see real improvements when doctors use precision medicine. This approach gives you treatments that match your genetic profile, environment, and lifestyle. You get care that fits you, not just the average patient. Doctors can predict how you will respond to certain therapies, which means you have a higher chance of success.
Studies show that precision medicine can improve response rates and progression‑free survival in cancer, and can also improve control of chronic conditions like hypertension and diabetes when treatments are tailored to individual risk profiles.
You notice that precision medicine gives you a much higher response rate and longer progression-free survival, especially in cancer care. You also see better control of blood pressure and diabetes. Doctors match treatments to your genetic changes, which leads to:
Studies consistently show higher objective response rates with genomically matched therapies compared with non‑matched treatment.
Matched therapies generally provide modest improvements in progression‑free survival compared with standard treatment.
Some long‑term survival benefits have been observed in genomically guided treatment cohorts, depending on cancer type.
You benefit from these improvements because your treatment works better and lasts longer.
Fewer Side Effects
Precision medicine helps you avoid many side effects. Doctors use genetic testing to find out how your body handles medicine. They adjust your dose or choose a drug that fits your genes. This reduces the risk of harmful reactions.
You get safer care because doctors can predict how you will react to medicine before you take it.
Here is a table that shows the difference between traditional medicine and genomically tailored therapies:
Aspect | Traditional Medicine | Genomically Tailored Therapies |
|---|---|---|
Risk of Adverse Effects | High | Low |
Treatment Effectiveness | Variable | High |
Patient Outcomes Improvement | 85% better | Significant reduction in side effects |
You experience fewer side effects and better results. Doctors use biomarkers and pharmacogenomics to personalize your treatment. This means you get medicine that works for you and does not cause unnecessary harm. You feel healthier and safer with precision medicine.
Applications in Healthcare
Cancer Care
You see the biggest impact of precision medicine in cancer care. Doctors use your genetic profile to choose treatments that target the mutations in your cancer cells. This approach has changed the lives of many patients. For example, targeted therapies for Chronic Myeloid Leukemia (CML) have turned a once fatal disease into a manageable condition. You benefit from genomically-matched treatments, which lead to better outcomes and fewer side effects.
Targeted therapies for CML improve survival rates and quality of life.
The IMPACT trials show that matching treatments to your genes leads to higher response rates.
The ISPY2.2 trial achieved a 65% complete response rate in immune-responsive breast cancer.
In large precision‑oncology programs, genomically matched therapies have shown higher response rates, modestly longer progression‑free survival, and better long‑term survival than non‑matched treatments.
Doctors use your genetic information to select therapies that work best for you. You get a higher chance of success and longer survival.
Rare Disease Treatment
Precision medicine gives you hope if you have a rare disease. Doctors use your genetic data to find the cause of your condition and select targeted therapies. Traditional treatments often fail for rare diseases, but precision medicine offers new options.
Disease | |
|---|---|
Duchenne muscular dystrophy | Gene therapies like ataluren and one-time gene therapy from Sarepta Therapeutics. |
Cystic fibrosis | CFTR modulators, including Trikafta, which can reverse effects of 178 mutations. |
PMM2-CDG | Drug repurposing studies identified epalrestat as a potential therapy. |
ADNP syndrome | Rational therapeutic design identified low-dose ketamine as a potential therapy. |
You benefit from these advances because doctors tailor treatments to your unique genetic makeup. This approach improves treatment effectiveness and reduces side effects.
Precision medicine helps doctors diagnose rare diseases faster and choose therapies that fit your needs.
Pharmacogenomics
Pharmacogenomics studies how your genes affect your response to medicine. Doctors use this information to prescribe drugs that work best for you and avoid harmful reactions.
Your genetic profile can change how you metabolize drugs like codeine or mercaptopurine.
Doctors test for gene variants, such as CYP2D6 or TPMT, before prescribing certain medicines.
Personalized prescriptions improve safety and effectiveness.
You receive medicine that matches your genes, which means you get better results and fewer side effects. Pharmacogenomics helps doctors make smarter choices for your care.
Challenges and Limitations
Cost and Access
You may notice that precision medicine is not available to everyone. The high cost of genetic testing and advanced diagnostics can make it hard for many people to benefit from these new treatments. For example, comprehensive tumor profiling and laboratory testing can cost over $20,000 per patient. This price can be even higher for rare diseases, where the cost-effectiveness is difficult to measure.
You also face challenges if you live in a region with limited healthcare resources. Many advanced tests and treatments are only available in a few countries. In places like Egypt, the high cost of genetic testing for breast cancer screening limits access for many patients. Even in wealthier countries, most resources are concentrated in large cities, leaving rural areas behind.
Genomic sequencing and advanced diagnostic tools often cost too much for many patients.
Personalized treatments can create financial barriers.
Geographic disparities limit access to precision medicine.
Socioeconomic factors make it harder for low-income patients to get advanced tests.
High-income patients are more likely to receive the latest imaging and diagnostic recommendations.
You may also see that only about 20% of precision medicine tests lead to cost savings. Many patients who get next-generation sequencing (NGS) testing cannot access the targeted drugs they need.
Ethics and Privacy
You might worry about how your genetic data is used and protected. Precision medicine raises important ethical questions. Safety is a concern, especially with new gene-editing tools that could have effects on future generations. Informed consent is another challenge, as it can be hard to explain all the risks, especially for treatments that affect future children.
Justice and equity matter, too. Some groups are underrepresented in genetic research, which means treatments may not work as well for everyone. Different countries have different rules for genome editing, which can lead to ethical dilemmas.
Aspect | Details |
|---|---|
Privacy Concerns | You may worry about misuse of your genetic information, which can affect your willingness to get tested. |
Legislative Action | Some countries, like Australia, Canada, and the UK, have laws to protect you from insurance discrimination based on genetic tests. |
Importance of Transparency | Clear rules about data storage and sharing help build trust in precision medicine. |
The General Data Protection Regulation (GDPR) sets rules for lawfulness, fairness, and transparency. It requires informed consent and limits how your data can be shared, helping protect your privacy.
You need to know that as precision medicine grows, new laws and policies will continue to shape how your data is used and protected.
You see how precision medicine uses your genetic, environmental, and lifestyle information to create treatments that fit you. The table below shows how this approach improves diagnosis, lowers costs, and empowers doctors.
Evidence Description | Impact on Healthcare Outcomes |
|---|---|
Precision medicine combines targeted therapies with personalized data. | Improves diagnosis and treatment efficacy. |
Utilizes genetic, clinical, and personal health data. | Achieves better health outcomes at potentially lower costs. |
Genetic testing enables quicker and more accurate cancer diagnoses. | Minimizes time on ineffective therapies and reduces harm. |
Engages patients holistically beyond medical records. | Enhances understanding of treatment efficacy and care outcomes. |
Combines art and science in medicine. | Reduces care variation and empowers clinicians. |
Requires comprehensive implementation across healthcare systems. | Advances clinical efficacy and optimizes care delivery. |
You benefit from better outcomes and safer care. Precision medicine continues to grow. Experts see new directions ahead:
Develop evidence of precision medicine’s effect.
Accelerate clinical data integration and assessment.
Promote integration of molecular guidance into care.
Develop innovation-oriented reimbursement and regulatory frameworks.
Strengthen engagement and trust of the public.
You face challenges such as privacy, ethics, and education. These issues include:
Ethical concerns about consent and data interpretation.
Patient education gaps.
Privacy issues with genetic information.
Cultural sensitivity and trust.
The need for diverse representation in studies.
You play a key role in the future of precision medicine. This approach promises safer, more effective care for everyone.
FAQ
What is the main goal of precision medicine?
You get care that matches your unique genetic makeup, environment, and lifestyle. Precision medicine aims to give you the best treatment for your needs, not just what works for most people.
How do doctors use your genetic information?
Doctors look at your genes to find changes that may affect your health. They use this information to choose treatments that work best for you and to avoid medicines that could cause side effects.
Is precision medicine only for cancer?
No, you can benefit from precision medicine in many areas. Doctors use it for rare diseases, heart conditions, and even to choose the right medicine for you.
Will your personal data stay private?
You have rights to your genetic data. Laws protect your privacy. Doctors and labs must keep your information safe and use it only for your care.
Can everyone access precision medicine?
You may face barriers like high costs or limited access in some areas.
Some hospitals and clinics offer more advanced tests than others.
Access depends on where you live and your healthcare coverage.
This article is for educational purposes only and is not a substitute for professional medical advice. For more details, please see our Disclaimer. To understand how we create and review our content, please see our Editorial Policy.
See Also
Choriocarcinoma: An Overview of Its Treatment Options
B-Cell Prolymphocytic Leukemia: A Simplified Explanation
Adamantinoma: Understanding Its Impact on the Body

