Pediatric Cancer Research Advances in 2026
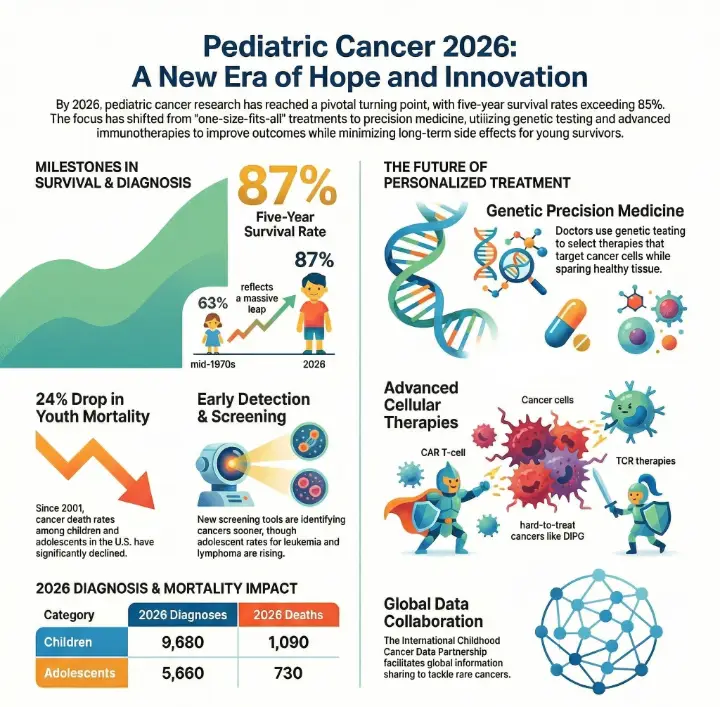
You witness exciting progress in the fight against childhood cancer in 2026. The five-year survival rate for children with cancer now exceeds 85%, and cancer death rates among youth in the U.S. have dropped by 24% since 2001. Scientists focus on early detection, prevention, and personalized care for each young patient. Increased funding and strong partnerships drive these changes. With the Spotlight on Pediatric Cancer Research and New Initiatives, you see hope rising and lives changing for families everywhere.
Key Takeaways
The five-year survival rate for children with cancer has increased to over 85%, showing significant progress in treatment.
Early detection and prevention are crucial; new screening tools help doctors find cancer sooner, leading to better outcomes.
Personalized therapies target each child's unique cancer, reducing side effects and improving recovery rates.
Collaboration among research institutions accelerates the development of new treatments, making them available to patients faster.
Ongoing funding is essential for pediatric cancer research; support from organizations and advocacy can drive future breakthroughs.
Spotlight on Pediatric Cancer Research and New Initiatives

Early Detection and Prevention Focus
You see a shift in how doctors and researchers approach pediatric cancer. Early detection and prevention now stand at the center of the Spotlight on Pediatric Cancer Research and New Initiatives. You learn that new screening tools help doctors find cancer sooner, which leads to better outcomes. Researchers track cancer rates and patterns in children and adolescents. They notice that cancer rates decline in children but rise in adolescents, especially for leukemia and lymphoma.
You can understand the impact of these trends by looking at the numbers:
Category | |
|---|---|
Children diagnosed with cancer | 9680 |
Adolescents diagnosed with cancer | 5660 |
Deaths in children | 1090 |
Deaths in adolescents | 730 |
Overall cancer diagnosis rate | 1 in 266 individuals before age 20 |
Common cancers in children | Leukemia, CNS tumors |
Common cancers in adolescents | CNS tumors, lymphoma, leukemia, thyroid cancer |
Trends in cancer rates | Decline in children, rise in adolescents due to leukemia and lymphoma |
You see that researchers use this data to create prevention programs and improve early detection. They focus on common cancers like leukemia and CNS tumors. You notice that Penn State teams work with partners such as Beat Childhood Cancer Research Consortium, Four Diamonds, and Targepeutics. Together, they develop new immunotherapies and launch clinical trials for hard-to-treat cancers like DIPG. These collaborations help bring new treatments to young patients faster.
Collaboration Partners | Focus Area | Expected Outcome |
|---|---|---|
Beat Childhood Cancer Research Consortium, Four Diamonds, Targepeutics | Development of GB13 immunotherapy for DIPG | Initiation of Phase I/II clinical trials for pediatric patients |
Personalized and Targeted Therapies
You discover that personalized medicine changes how doctors treat pediatric cancer. The Spotlight on Pediatric Cancer Research and New Initiatives highlights new ways to match treatments to each child’s unique cancer. Doctors use genetic tests to learn about the cancer’s makeup. They select therapies that target the cancer cells while sparing healthy cells. This approach helps reduce side effects and improves recovery.
You see Penn State researchers lead clinical trials that test these targeted therapies. They work with national partners and use federal funding to support their studies. You learn that grants from the NIH and NCI make these trials possible. Programs like the Childhood Cancer STAR Act and the Childhood Cancer Data Initiative receive support from NCI funding. These programs help researchers collect data, develop new treatments, and improve survivorship care.
Federal funding plays a key role in advancing pediatric cancer research:
Federal funding is essential for innovative research and development in pediatric cancer due to limited incentives for drug companies.
Research institutions depend on grants from NIH and NCI to discover new treatments and cures.
Programs like the Childhood Cancer STAR Act and the Childhood Cancer Data Initiative are supported by NCI funding, ensuring progress in research and survivorship care.
You notice that the U.S. Department of Health and Human Services doubled funding for the Childhood Cancer Data Initiative from $50 million to $100 million. This increase helps researchers develop better diagnostics, treatments, and prevention strategies. The initiative collects and analyzes childhood cancer data, which improves research outcomes and helps doctors make informed decisions.
Advances in Cellular and Immunotherapies
You witness exciting progress in cellular and immunotherapies in 2026. The Spotlight on Pediatric Cancer Research and New Initiatives brings attention to smarter T-cell therapies and innovative combinations that boost treatment success. Doctors use CAR T-cell therapy, tumor-infiltrating lymphocyte (TIL) therapies, and T-cell receptor (TCR) transduced T cells to fight cancer.
Experts predict smarter cell therapies that can operate in challenging environments.
Anticipated advancements include T-cell therapies, tumor-infiltrating lymphocyte (TIL) therapies, and T-cell receptor (TCR) transduced T cells.
You learn that current CAR T-cell trials have not fully used enhancements for multi-specificity and T cell potency. Future studies will test these therapies earlier in the disease course. Combinatorial regimens that include cell therapies are expected to improve outcomes for young patients.
Current CAR T-cell trials have not fully utilized enhancements for multi-specificity and T cell potency.
Future studies are expected to test these therapies earlier in the disease course.
Combinatorial regimens incorporating cell therapies are anticipated.
You see that the Center for Excellence in Pediatric Immuno-Oncology (CEPIO) helps translate lab findings into clinical applications. This collaboration improves treatment efficacy and brings hope to families. You read about successful CAR T-cell therapy administered to a patient in clinical trials at St. Jude, showing how immunotherapy advances help children with cancer.
Evidence Type | Description |
|---|---|
CAR T-cell Therapy | Successful CAR T-cell therapy was administered to a patient in clinical trials at St. Jude, showcasing advancements in immunotherapy for pediatric cancer. |
Collaborative Efforts | The Center for Excellence in Pediatric Immuno-Oncology (CEPIO) facilitates the translation of lab findings to clinical applications, enhancing treatment efficacy. |
You realize that these advances in cellular and immunotherapies offer new options for children and adolescents. The Spotlight on Pediatric Cancer Research and New Initiatives shows you how research, collaboration, and funding drive progress in early detection, personalized treatments, and innovative therapies.
Survival and Treatment Outcomes
Trends in Pediatric Cancer Survival
You see remarkable progress in survival rates for children with cancer. Over the past decades, the five-year survival rate for all pediatric cancers combined has increased from 63% in the mid-1970s to 87% in recent years. According to the AACR Pediatric Cancer Progress Report 2025, this upward trend continues. Children who once had few options now benefit from new treatments and better care. However, you should know that among children who survive five years after diagnosis, about 18% may face life-threatening health issues within the next 25 years. This fact highlights the need for ongoing research and support.
Five-year survival rate rose from 63% (1970s) to 87% (2015-2021)
18% of five-year survivors may die within 25 years post-diagnosis
Survival rates keep improving with new therapies
Reducing Side Effects and Improving Quality of Life
You learn that new treatments do more than save lives. They also help reduce side effects and improve quality of life for survivors. Researchers now use prediction models to find children at risk for serious late effects, such as kidney failure. Doctors use cardiac biomarkers to spot survivors at risk for heart problems. These tools allow for more tailored care and better monitoring. Targeted therapies and personalized survivorship care plans help children and families manage long-term health. Over 90% of children with acute lymphoblastic leukemia (ALL) are cured, but about 20% may develop chronic health conditions later. Survivorship guidelines and care plans help you understand and manage these risks.
Personalized survivorship care plans address unique needs
Cardiac biomarkers help identify risk for heart problems
Guidelines support long-term health and quality of life
Addressing Survival Inequalities
You notice that not all children have the same chance of survival. Survival rates vary by region and access to care. For example, the five-year survival rate in China is 77.2%. In high Socio-demographic Index (SDI) regions, the rate is 84.9%, while in low SDI regions, it drops to 72.6%. Adolescents face greater disparities, especially with cancers like leukemia and lymphoma. Children who travel for care may see an 18.2% difference in survival compared to those treated closer to home. The Spotlight on Pediatric Cancer Research and New Initiatives brings attention to these gaps and encourages efforts to close them.
Region/Group | Five-Year Survival Rate |
|---|---|
High SDI regions | 84.9% |
Low SDI regions | 72.6% |
China (overall) | 77.2% |
Adolescents (low SDI) | Lower than children |
Patients traveling for care | 18.2% lower |
You play a role in raising awareness and supporting research that aims to give every child the best chance at survival and a healthy future.
Ongoing Challenges in Pediatric Cancer
Funding and Research Gaps
You face major challenges in pediatric cancer research because of funding cuts. The National Cancer Institute (NCI) funding drops by 37%, from $7.22 billion to $4.53 billion. This is the lowest level since 2002. You see over 1,000 fewer research grants and a reduction in research centers from 27 to just 5. Key programs like the Pediatric Brain Tumor Consortium and the Pediatric Early-Phase Clinical Trial Network lose 21% of their funding, totaling $127.9 million. Intramural research loses $484.4 million, a 36% reduction. Training awards for new scientists are slashed by 37.4%. These cuts threaten the future of cancer research and limit the number of new discoveries.
Funding limitations slow the development of new treatments. You notice that researchers struggle to start new projects or continue promising studies. The 2026 appropriations process shows how important it is to secure enough funding. When lawmakers reject budget cuts and support federal funding, you see progress in creating new therapies for children.
Rare and Hard-to-Treat Cancers
You learn that rare and hard-to-treat cancers present unique obstacles. Small patient populations make clinical trials difficult. For example, cancers like ETMR and ATRT have very few patients, so researchers cannot easily test new treatments. Ethical concerns also arise because children are vulnerable, and consent can be complicated. Funding and incentives for rare diseases remain limited, even with laws like the Creating Hope Act and RACE Act. You also see that a lack of research cooperation leads to missed opportunities. When teams do not work together, progress slows for these challenging cancers.
Access to Care and Disparities
You notice that not every child has the same chance to survive cancer. In high-income countries, survival rates reach 80%. In low-income and lower-middle-income countries, survival rates stay below 30%. Differences in healthcare infrastructure and economic development affect access to treatment. Timely diagnosis and supportive care are critical for better outcomes. In the United States, Latino children have the highest uninsured rates. Black and Latino children without insurance face worse cancer outcomes than other groups. These disparities show why you must support efforts to improve access and equity in pediatric cancer care.
Future Directions and Research Priorities
Innovative Clinical Trials in 2026
You see new clinical trials changing the way doctors treat childhood cancer. These trials use flexible designs and new methods to help more children. Researchers use existing data and Bayesian statistics to make trials faster and more accurate. This helps when there are only a few patients with rare cancers. You notice that these changes make trials less expensive and easier to run.
Treatment | Description | Status |
|---|---|---|
Revumenib | Used for relapsed or refractory AML in children as young as 1. | Ongoing studies for long-term results. |
CAR T-Cell Therapy | Targets GD2 in brain tumors. | More Phase I/II studies planned. |
Dordaviprone | Treats H3 K27M-mutant diffuse midline glioma. | Needs Phase III trials. |
Selumetinib | Helps children with NF1 tumors. | Expanded use after Phase II success. |
Aspect | Description |
|---|---|
Use existing data to help with small patient groups. | |
Bayesian Methodologies | Build on past results for better planning. |
Cost and Feasibility | Make trials easier and cheaper for rare diseases. |
Global Collaboration and Advocacy
You see experts from around the world working together. The National Cancer Institute and the French National Cancer Institute led a big meeting in Paris. Over 200 experts joined to share data and ideas. They started the International Childhood Cancer Data Partnership. This group collects information from many countries to help doctors learn more about rare cancers. The G7 Cancer group also works on new ways to share data and improve care.
International advocacy has played a significant role in shaping pediatric cancer research priorities in 2026, particularly through initiatives like the WHO Global Initiative for Childhood Cancer. This initiative emphasizes collaboration among governments, healthcare providers, and advocacy groups to improve childhood cancer care and outcomes globally.
Focus on Adolescent and Young Adult Care
You learn that teenagers and young adults with cancer have special needs. Cancer can disrupt school, work, and future plans. Many survivors face health problems later in life. Only half of young adults talk about fertility with their doctors before treatment. Many want to discuss their goals, like education and family planning.
Initiative | Focus Area | Goals |
|---|---|---|
Care of AYAs with Cancer in Low-Resourced Countries | Find barriers, create solutions, write guidelines, train doctors | |
BRIDGE Program | Early-onset cancer care | Support, early fertility counseling, genetic testing, education |
Develop guidelines for care that fit local resources.
Train healthcare workers to meet the needs of young people.
Find new ways to help young patients get quick diagnosis and treatment.
You see that research now focuses on helping young people live healthy, full lives after cancer.
You see major progress in pediatric cancer research in 2026. New treatments like targeted therapies and immunotherapies, better early detection tools, and global teamwork help more children survive and live better lives.
Five-year survival rates now reach up to 88%.
Projects like Project:EveryChild and new AI tools improve diagnosis and care.
Community support and funding drive these breakthroughs.
Priority | Impact |
|---|---|
Innovative Research | Brings new hope for cures |
Equitable Care | Gives every child a fair chance |
Survivorship | Supports long-term health and well-being |
You play a key role in this journey. Your support brings hope for every child and family facing cancer.
FAQ
What are the most common types of pediatric cancer?
You see leukemia, brain and central nervous system tumors, and lymphoma as the most common types.
Doctors often treat leukemia first because it affects blood and bone marrow.
How do new treatments improve survival rates?
You benefit from targeted therapies and immunotherapies. These treatments attack cancer cells directly.
Fewer side effects
Higher survival rates
Better quality of life
Why is early detection important?
You get a better chance at recovery when doctors find cancer early. Early detection helps doctors start treatment sooner.
Early diagnosis often leads to improved outcomes and fewer complications.
How can you support pediatric cancer research?
You can donate, join awareness campaigns, or volunteer.
Action | Impact |
|---|---|
Donate | Funds new research |
Volunteer | Supports families |
Share | Raises awareness |
This article is for educational purposes only and is not a substitute for professional medical advice. For more details, please see our Disclaimer. To understand how we create and review our content, please see our Editorial Policy.
See Also
Exploring Symptoms And Treatments For Conjunctival Melanoma
Recognizing Symptoms And Treatment Options For Duodenal Cancer
An In-Depth Overview Of Various Cancer Types Available
Essential Symptoms, Diagnosis, And Treatment Insights For LGL Leukemia

